Index
This topic area covers statistics and information relating to mental health and emotional wellbeing among children and young people in Hull including local strategic need and service provision. Further information relating to Mental Health and Emotional Wellbeing Among Adults is given under Health Factors within Adults. Further information on Learning Disabilities, Mental Ill Health and Children with Special Educational Needs or Disabilities is provided under Vulnerable Groups. Information relating to hospital admissions for self-harm, alcohol and substance use can be found within A&E Attendances and Hospital Admissions under Health Factors under Children and Young People. More information on mental health and emotional wellbeing and early intervention is also available under Early Help and Prevention Programme under Child Development within Children and Young People.
Emotional wellbeing, bullying, frequency of worrying about different things, and feelings of safety have all been collected within Hull’s Young People Health and Wellbeing Surveys. This page contains information collected in the latest 2024 Young People Health and Wellbeing Survey.
This page contains information from the Office for Health Improvement & Disparities’ Fingertips. Information is taken ‘live’ from the site so uses the latest available data from Fingertips and displays it on this page. As a result, some comments on this page may relate to an earlier period of time until this page is next updated (see review dates at the end of this page).
Summary Infographic

Headlines
- Health Needs Assessments have been completed in Hull for emotional wellbeing and mental health among young people in 2023, and among pre-school children in 2022.
- From the local Young People Health and Lifestyle Survey 2024 which involved almost 4,000 pupils attending eight of Hull’s 13 main-stream secondary schools, 47% reported good or very good mental health, but 27% reported poor or very poor mental health. Just over one-quarter (28%) had been bullied in the last year and almost all children (93%) had an adult to talk to if things were bothering them. Three-quarters of young people felt safe in their local area.
- At the time of the survey, it was estimated that 17,376 secondary school age young people lived in Hull, and this would equate to around 8,199 young people with good or very good mental health, 4,704 with poor or very poor mental health and 4,792 having been bullied in the last year.
- There were relatively small differences in the percentage who had good or very good mental health across the school years, but marked differences between males and females. Overall, 59% of males reported good or very good mental health compared to 38% of females. Young people who were LGBTQ+ and young people whose daily activities were limited by long-term illness or disability had much lower percentages reporting good or very good mental health (28% and 38% respectively).
- Around one in five males in school years 7 (aged 11-12 years) to 10 (aged 14-15 years) reported poor or very poor mental health, but this was higher at 29% among males in Year 11 although there is uncertainty around the findings among males in Year 11 as the numbers surveyed are relatively low. Females had much higher levels of poor or very poor mental health at 27% among those in Year 7 increasing to 35% among those in Year 10 before falling slightly to 33% in Year 11. Levels of poor or very poor mental health were much higher among young people who were LGBTQ+ (45%) and young people whose daily activities were limited by long-term illness or disability (44%).
- Young people worried most about how they looked with 27% worrying about this a lot and 17% worrying about this quite a lot. They also worried most frequently about family (43%), relationships and friends (42%), school tests and exams (39%), money (35%), their weight (33%) and someone else’s health (30%). Younger pupils were more likely to worry about most of the life factors that they were asked about with the exception of money, school tests and exams, and getting a job. Females were also more likely to worry about things compared to males. Four in ten young people living in the most deprived fifth of areas of Hull worried a lot or quite a lot about money compared to just over one-quarter (26%) of young people living in the least deprived fifth of areas of Hull.
- Females were more likely to state they had been bullied in the last year compared to males (31% versus 24%), and Year 7 pupils were more likely to have experienced bullying compared to Year 11 pupils for both males (34% of Year 7 males, 17% for Year 10 males and 22% for Year 11 males) and females (35% of Year 7 females, 38% of Year 8 females and 21% of Year 11 females).
- Young people who were LGBTQ+ (46%) and young people whose daily activities were limited by long-term illness or disability (44%) were much more likely to have been bullied in the last year. As a consequence, young people who were LGBTQ+ (32%) and young people whose daily activities were limited by long-term illness or disability (26%) were much more likely to worry a lot or quite a lot about bullying compared to 17% overall.
- Eight in ten of those who had been bullied in the last year stated that it had occurred at school (81%) with 26% occurring not at school but by a pupil from school, 22% on the way to or from school, and 14% by someone else not at school. One-third had been bullied on social media, 9% had been bullied at home, and 15% reported being bullied somewhere else. Over three-quarters of bullying was name-calling and teasing, 60% was having lies or rumours spread about them, and 56% were bullied in relation to their appearance.
- Seven in ten would tell a parent or carer if they were bullied, 40% would tell a friend, 36% would tell someone at school and 30% would tell another family member. Overall, 8% stated they would tell no-one, and 7% stated they didn’t know if they would tell anyone.
- Over nine in ten of young people had someone to talk to if things were bothering them, although if the young people who stated they didn’t know were included then around 10% of males in Years 7 to 10 stated they had no-one to talk to or didn’t know increasing to 29% for Year 11 males. For females, the percentages varied between 16% and 21% between the school years and was 17% overall. Whilst the percentage is high for Year 11 males, there is uncertainty around the estimate given the relatively small number of Year 11 males that participated in the local survey.
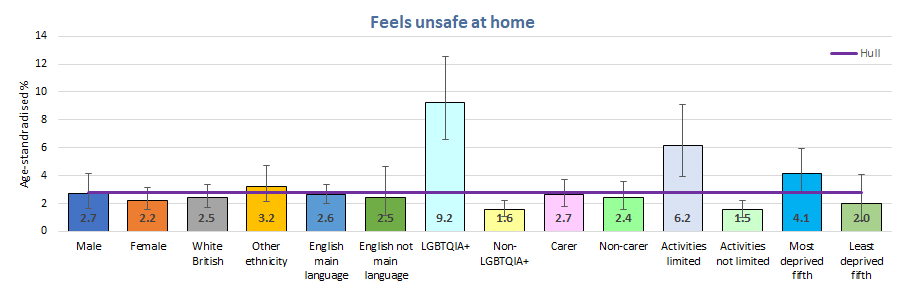
- Over 95% of young people surveyed in the local Health and Wellbeing Survey in 2024 felt safe at home. Overall, 2.7% of males and 2.2% of females felt very unsafe or a bit unsafe at home, but this was considerably higher among young people who were LGBTQ+ (9%), and young people whose daily activities were limited by long-term illness or disability (6%). Around three-quarters of young people felt safe in their local area, over two-thirds felt safe at school, almost six in ten males and around half of females felt safe in the local park and in Hull city centre, and over three-quarters of males and females felt safe online although the percentages increased with age with females. Young people who were LGBTQ+ and young people whose daily activities were limited by long-term illness or disability were more likely to feel unsafe at home, in the local area, at school and in Hull city centre, but there was no real differences for them for feelings of safety in the local park and feelings of safety whilst online.
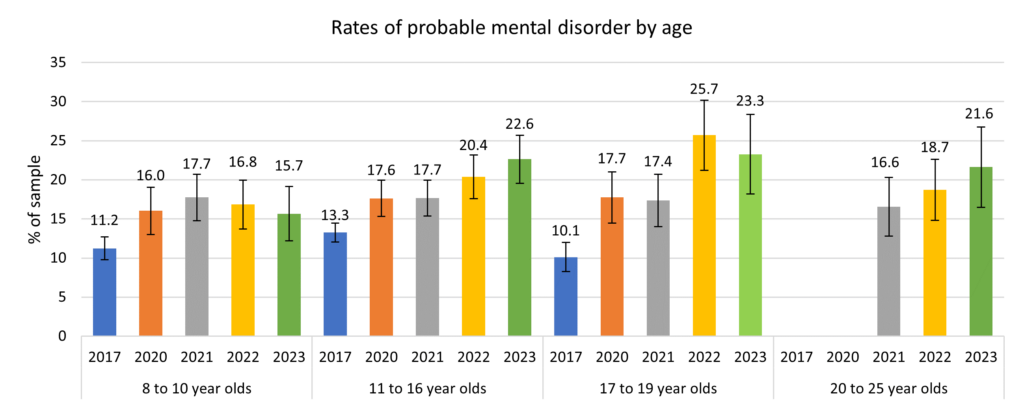
- From the Mental Health of Children and Young People in England survey in 2023, it is estimated that 15.7% of 8-10 year olds, 22.6% of 11-16 year olds, 23.3% of 17-19 year olds and 21.6% of 20-25 year olds have a probable mental health disorder in England. The percentages have risen sharply since 2017. The prevalence estimates for young people in England were lower among females aged 8-10 years compared to males, but the reverse was true for older ages. Using these prevalence estimates from England for 2023, out of the 63,705 children and young people aged 8-25 years estimated to live in Hull in 2024, it is estimated that 13,472 have a probable mental health disorder. The report also represents some stark information in relation to the impact and consequence of factors such as poverty, illness, worklessness and homelessness in relation to mental health with a much higher percentage of young people with probable mental health facing multiple, overlapping challenges rooted in poverty, instability and inequality. As Hull is among the most deprived local authorities in England, it is therefore likely that the total number of young people estimated to have a probable mental health condition in Hull based on national prevalence estimates is an under-estimate of the true number.
- From the Mental Health of Children and Young People in England survey in 2023, it is estimated that 2.6% of 11-16 year olds, 12.5% of 17-19 year olds and 5.9% of 20-25 year olds have an eating disorder. Using these prevalence estimates from England for 2023, out of the 53,096 children and young people aged 11-25 years estimated to live in Hull in 2024, it is estimated that 3,143 have an eating disorder.
- Children and young people who are LGBTQ+, living in poverty, have adverse childhood experiences, who live with a parent with poor mental health, have recognised special educational needs or disabilities, are excluded from school, have poor housing, are being looked after or are leaving or have left care, who are a young carer and/or who are experiencing bereavement all have higher levels of poor mental health and emotional wellbeing. Many of these factors are present together which compound and magnify poor mental health and emotional wellbeing.
- For 2023/24, just under half of children (48%) who were looked after in Hull had a strengths and difficulties questionnaire score that was of concern in Hull compared to 41% for England. The percentage in Hull was statistically significantly higher than England, although for the years 2015/16 to 2022/23, the percentage in Hull has been comparable or lower than England, and 2023/24 is the first year that the percentage in Hull has been significantly higher than England.
- The COVID-19 pandemic and likely subsequent cost of living crisis has impacted detrimentally on mental health and emotional wellbeing among young people, and referrals into Children and Young People Mental Health Services at a national level have increased dramatically in the last few years. In the Centre for Young Lives’ 2025 State of Childhood Vulnerability report, which was published in July 2025, they warn that the COVID-19 pandemic is still casting a long shadow over millions of children in England five years on. They also present statistics illustrating that the circumstances facing children and young people have deteriorated in relation to deprivation, poverty, financial resilience, homelessness, school absence, special educational needs, autism, mental health, not in education, training or employment, and violence. Factors which all have a detrimental impact on mental health and emotional wellbeing. Societal changes in the last few years in relation to social media is considered to adversely affect children and young people’s mental health and emotional wellbeing.
The Population Affected – Why Is It Important?
World Health Organisation (WHO) state that mental health is an integral and essential component of health. The WHO constitution states: “Health is a state of complete physical, mental and social well-being and not merely the absence of disease or infirmity.” An important implication of this definition is that mental health is more than just the absence of mental disorders or disabilities.
WHO state mental health is a state of well-being in which an individual realises his or her own abilities, can cope with the normal stresses of life, can work productively and is able to make a contribution to his or her community. Mental health is fundamental to our collective and individual ability as humans to think, emote, interact with each other, earn a living and enjoy life. On this basis, the promotion, protection and restoration of mental health can be regarded as a vital concern of individuals, communities and societies throughout the world.
They go on to say that multiple social, psychological, and biological factors determine the level of mental health of a person at any point of time. For example, violence and persistent socio-economic pressures are recognized risks to mental health. The clearest evidence is associated with sexual violence. Poor mental health is also associated with rapid social change, stressful work conditions, gender discrimination, social exclusion, unhealthy lifestyle, physical ill-health and human rights violations. There are specific psychological and personality factors that make people vulnerable to mental health problems. Biological risks include genetic factors.
Thus poor mental health can have a detrimental effect on all aspects of life undermining self-esteem, confidence and enthusiasm for life. Social and emotional well-being in children creates the foundations for healthy behaviours and educational attainment. It also helps prevent other things like substance use and mental health problems. Social and emotional well-being provides personal competencies (such as emotional resilience, self-esteem and interpersonal skills) that help to protect against risks relating to social disadvantage, family disruption and other adversity in life. Such competencies provide building blocks for personal development which will enable children and young people to take advantage of life chances.
Evidence shows that poor social and emotional wellbeing predicts a range of negative outcomes in adolescence and adulthood. The National Institute for Health and Care Excellence state that negative parenting and poor quality family or school relationships place children at risk of poor mental health. Early intervention in childhood can help reduce physical and mental health problems and prevent social dysfunction being passed from one generation to the next.
A general low mood can include sadness, anxiety, worry, tiredness, low self-esteem, frustration and anger and people with poor mental health sometimes can deal with this by smoking more, eating excessively and unhealthy diets and not exercising. Depression can involve continuous low mood, feelings of hopelessness and helplessness, low self-esteem, feeling tearful, feeling irritable and intolerant of others, having no motivation of interest in things, finding it difficult to make decisions, not getting any enjoyment out of life, having suicidal thoughts or thoughts of self-harming, and feeling anxious or worried. As a consequence, poor mental health influences all aspects of life, a person’s physical health, their family, their education and training, their workplace and employment, and their involvement in their community.
In recent years, there has been increasing acknowledgement of the important role mental health plays in achieving global development goals, as illustrated by the inclusion of mental health in the Sustainable Development Goals. Depression is one of the leading causes of disability. Suicide is the second leading cause of death among 15-29-year-olds. People with severe mental health conditions die prematurely – as much as two decades early – due to preventable physical conditions.
Despite progress in some countries, people with mental health conditions often experience severe human rights violations, discrimination, and stigma.
Many mental health conditions can be effectively treated at relatively low cost, yet the gap between people needing care and those with access to care remains substantial. Effective treatment coverage remains extremely low.
Increased investment is required on all fronts: for mental health awareness to increase understanding and reduce stigma; for efforts to increase access to quality mental health care and effective treatments; and for research to identify new treatments and improve existing treatments for all mental disorders. In 2019, WHO launched the WHO Special Initiative for Mental Health (2019-2023): Universal Health Coverage for Mental Health to ensure access to quality and affordable care for mental health conditions in 12 priority countries to 100 million more people.
Mental health conditions are increasing worldwide. Mainly because of demographic changes, there has been a 13% rise in mental health conditions and substance use disorders in the last decade (to 2017). Around 20% of the world’s children and adolescents have a mental health condition, with suicide the second leading cause of death among 15-29-year-olds. Approximately one in five people in post-conflict settings have a mental health condition.
Mental health conditions can have a substantial effect on all areas of life, such as school or work performance, relationships with family and friends and ability to participate in the community. Two of the most common mental health conditions, depression and anxiety, cost the global economy US$1 trillion each year. Mental Health First Aid estimates that mental health costs the UK economy £105 billion each year.
Despite these figures, the global median of government health expenditure that goes to mental health is less than 2%.
The Hull Picture
Needs Assessment 2023
A Health Needs Assessment Children and Young People Emotional Wellbeing and Mental Health was undertaken in March 2023.
Needs Assessment of Children Aged 2-4 Years 2022
A mini needs assessment on mental health was undertaken in 2022 for children aged 2-4 years in Hull.
Hull’s Young People Health and Wellbeing Survey 2024
Eight of Hull’s 13 main-stream secondary schools took part in Hull’s Young People Health and Wellbeing Survey between 6 March and 3 May 2024 with a total of 3,910 young people aged 11-16 years taking part. Further details can be found on Hull’s Young People Health and Wellbeing Surveys.
Young people were asked about bullying, if they had been treated unfairly, if they had good or poor mental health, if they had an adult to talk to as well as feelings of safety in their local area.
The prevalence estimates generally differed for males and females, and across the five school years, Year 7 (aged 11-12 years) to Year 11 (aged 15-16 years) so the age-standardised percentages were calculated which adjusted to account for the differences in the prevalence by age, and in effect give a summary measure over all age groups taking into account the total number of children living in Hull within those age ranges.
There were a small number of Year 11 boys surveyed so the results should be treated cautiously for this group.
The age-standardised percentages were as follows for some of the measures of mental health and emotional wellbeing:
- 47.2% had good or very good mental health.
- 27.1% had poor or very poor mental health.
- 27.6% had been bullied in the last year.
- 92.5% had an adult to talk to.
- 77.6% felt safe in their local area.
At the time of the survey analysis, the Office for National Statistics estimated that there were 17,376 secondary school age young people living in Hull (mid-year 2023 resident population estimates).
Using the above prevalence estimates and the estimated population, it was possible to estimate the total number of young people of secondary school age living in Hull on the basis of these mental health and emotional wellbeing measures:
- Out of an estimated 17,376 residents of secondary school age:
- 8,199 had good or very good mental health.
- 4,704 had poor or very poor mental health.
- 4,792 had been bullied in the last year.
- 16,072 had an adult to talk to.
- 13,484 felt safe in their local area.
Self-Reported Mental Health Status
Overall, males reported better mental health compared to females with a much higher percentage reporting very good or good health among males. Whilst more females reported their mental health was OK, higher percentages of females reported poor or very poor mental health.

The percentage with very good or good mental health were not drastically different across the five year groups for either males or females which ranged between 54% and 62% across the school years for males and between 35% and 42% for females.

A lower percentage of young people report very good or good mental health among those living in the most deprived fifth of areas of Hull (46%) compared to those who lived in the least deprived fifth of areas of Hull (52%) based on the Index of Multiple Deprivation 2019. However, the differences were not statistically significant.
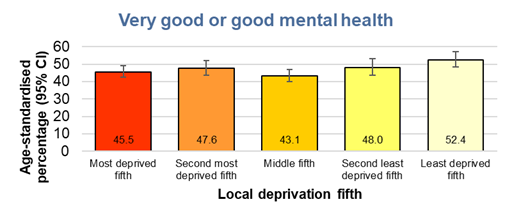
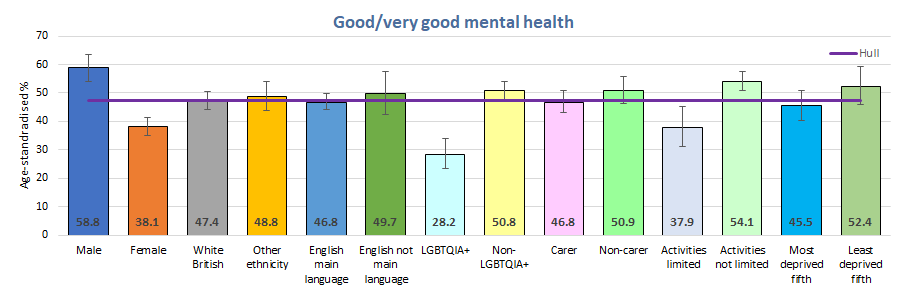
There were significant differences among different groups of young people in terms of the percentage who reported very good or good mental health. Males were much more likely to report very good or good mental health compared to females (59% versus 38%) and young people who were not LGBTQ+ compared to young people who were LGBTQ+ (51% versus 28%), and young people whose daily activities were not limited by long-term illness or disability compared to those whose activities were limited (54% versus 38%).
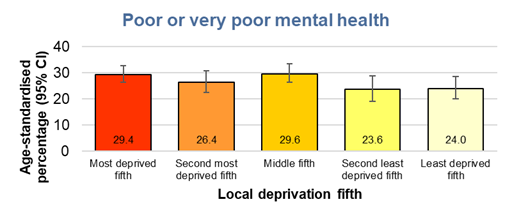
Around one in five males reported poor or very poor mental health with a slightly smaller percentage at 16% for Year 9s. The percentages were higher among Year 11 males at 29% although this is not known if it is a real factor or a consequence of the relatively small number of Year 11 males that participated the in the survey (the 95% confidence intervals are wide denoting uncertainty around the percentage). For females, the percentages reporting poor or very poor mental health were much higher at just under one-third of females overall. The percentages were lowest among Year 7 females at 27% before increasing for the older school years.

Not surprisingly, the reverse associations were present when examining the percentages who reported poor or very poor mental health where there has been differences between groups in relation to very good or good mental health.
Just under three in ten (29%) stated their mental health was poor or very poor among young people living in the most deprived fifth of areas of Hull compared to under one-quarter (24%) among young people living in the least deprived fifth of areas of Hull. However, the differences were not statistically significant.
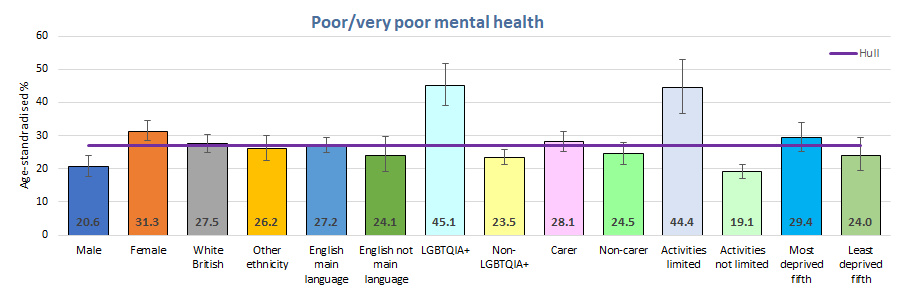
Almost one-third of females and around 45% of young people who were LGBTQ+ or whose daily activities were limited by long-term illness or disability reported poor or very poor mental health.
Worries
Young people most frequently worried about how they looked with 27% worrying about this a lot and 17% worrying about this quite a lot. They also worried about relationships and friends, family, school tests and exams, money, their weight, someone else’s health, getting a job, feeling lonely, their health, and their identity.
Fewer than 20% worried a lot or quite a lot about homework, pressure to do something they didn’t want to do, bullying, violence, gangs, staying safe online and climate change.

The table below illustrates the percentages of young people who worried a lot or quite a lot about these various aspects of life (ordered with the worries with the highest percentages at the top of the table) by school year for males and females separately.
The younger pupils were much more likely to worry about all these factors compared to the older pupils with the exception of money, school tests and exams, and getting a job. Females were more likely to worry a lot or quite a lot about most of these life issues compared to males although for some year groups males worried more than females in relation to money, getting a job and climate change. Year 11 males were more likely to worry a lot or quite a lot compared to Year 11 females. However, there were a small number of Year 11 boys surveyed so the results should be treated cautiously for this group.
Young people who had long-term illness or disabilities that limited their daily activities were more likely to worry a lot or quite a lot compared to all young people surveyed (see Physical Health Among Children and Young People).
| Worry | Male Y7 | Male Y8 | Male Y9 | Male Y10 | Male Y11 | Female Y7 | Female Y8 | Female Y9 | Female Y10 | Female Y11 |
| How I look | 33.6 | 28.5 | 27.8 | 30.3 | 24.2 | 55.1 | 62.6 | 56.1 | 65.1 | 44.2 |
| Relationships and friends | 38.9 | 33.3 | 33.7 | 30.0 | 37.3 | 53.9 | 56.0 | 48.7 | 48.0 | 44.9 |
| Family | 43.3 | 39.3 | 37.8 | 38.7 | 45.3 | 49.7 | 51.0 | 44.3 | 45.1 | 35.5 |
| School tests and exams | 33.6 | 27.6 | 27.1 | 30.3 | 57.1 | 40.9 | 41.9 | 41.1 | 54.1 | 67.0 |
| Money | 31.4 | 31.9 | 36.3 | 37.9 | 39.6 | 28.8 | 36.6 | 35.5 | 40.8 | 33.7 |
| My weight | 26.3 | 23.6 | 20.4 | 18.9 | 27.6 | 40.4 | 51.5 | 42.3 | 44.1 | 37.0 |
| Someone else’s health | 32.8 | 25.0 | 25.3 | 21.5 | 37.6 | 38.1 | 32.8 | 34.9 | 29.5 | 26.3 |
| Getting a job | 27.4 | 23.9 | 26.0 | 27.4 | 48.4 | 22.5 | 27.6 | 28.4 | 35.7 | 32.7 |
| Feeling lonely | 20.1 | 17.1 | 14.7 | 17.2 | 27.3 | 33.3 | 37.7 | 28.1 | 30.9 | 24.7 |
| My health | 23.3 | 21.2 | 16.9 | 18.0 | 25.2 | 27.4 | 31.5 | 25.9 | 27.5 | 22.2 |
| My identity | 18.6 | 16.3 | 14.6 | 15.3 | 14.5 | 24.6 | 27.8 | 19.7 | 20.3 | 17.1 |
| Homework | 22.6 | 19.0 | 15.3 | 14.2 | 15.7 | 27.7 | 20.1 | 15.5 | 23.3 | 11.1 |
| Pressure to do something I don’t want to | 20.1 | 13.5 | 10.3 | 9.2 | 19.2 | 27.6 | 28.6 | 18.6 | 15.8 | 12.0 |
| Bullying | 18.3 | 15.8 | 13.2 | 12.6 | 16.6 | 26.1 | 25.7 | 17.1 | 17.3 | 6.0 |
| Violence | 18.0 | 13.8 | 10.9 | 11.0 | 14.2 | 19.9 | 25.0 | 14.3 | 13.1 | 6.3 |
| Gangs | 17.1 | 10.3 | 10.1 | 8.4 | 7.3 | 19.3 | 19.9 | 11.5 | 10.6 | 8.5 |
| Staying safe online | 15.7 | 11.0 | 8.5 | 7.1 | 11.5 | 16.8 | 13.9 | 9.9 | 7.1 | 2.6 |
| Climate change | 14.5 | 8.0 | 8.7 | 7.9 | 5.1 | 11.7 | 10.3 | 8.5 | 9.7 | 8.1 |
Young people living in the most deprived fifth of areas of Hull were more likely to worry a lot or quite a lot about money (41%) compared to young people living in the least deprived fifth of areas of Hull (26%) based on the Index of Multiple Deprivation 2019.
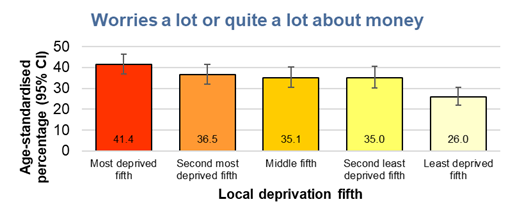
There were no differences in the percentages overall who worried a lot or quite a lot about money between the males (35.4%) and females (35.1%), although females living in the most deprived two-fifths of areas of Hull were more likely to worry a lot or quite a lot about money (44.2% in most deprived fifth and 40.1% in second most deprived fifth) compared to males (41.6% and 29.9% respectively), but males living in the least deprived three-fifths of areas of Hull were more likely to worry a lot or quite a lot about money (28.9% in least deprived fifth, 38.1% in second least deprived fifth and 38.1% in middle fifth) compared to females (23.8%, 32.7% and 31.9% respectively).
Bullying
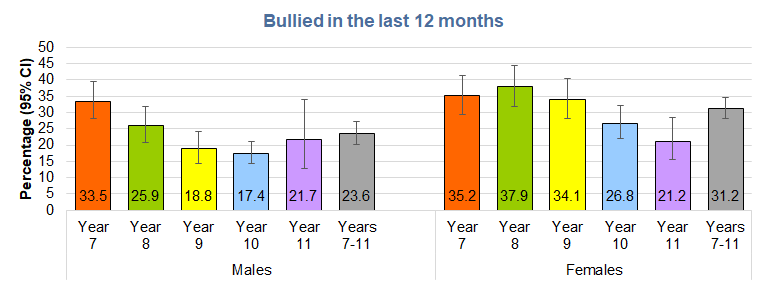
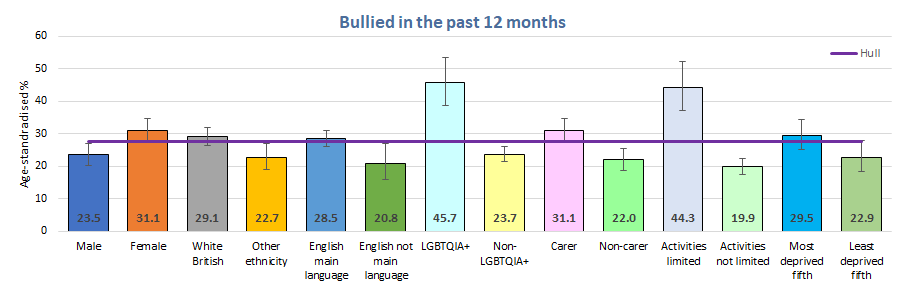
Overall, 27.6% had been bullied in the last year with the highest percentages among the younger school years with higher percentages among females (31.2%) compared to males (23.6%).
Younger pupils were much more likely to have experience bullying in the last year compared to older pupils. One-third of males in Year 7 had experienced bullying which decreased to 17% among males in Year 10, and the percentage was slightly higher among males in Year 11 at 22%. Among females, 35% in Year 7 and 38% in Year 8 had experienced bullying in the last year which fell to 21% among females in Year 11.
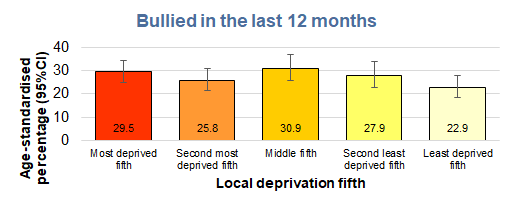
Young people who were living in the most deprived fifth of areas of Hull based on the Index of Multiple Deprivation 2019 reported slightly higher percentages of bullying, although the differences were percentages for the most and least deprived fifths were not statistically significantly different compared to the Hull average.
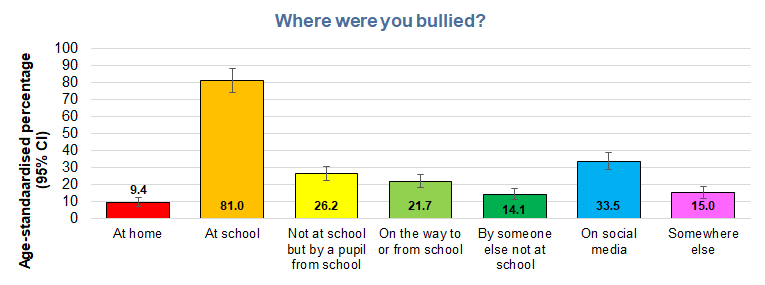
The majority of the bullying occurred at school with eight in ten cases of bullying occurring at school. A further quarter of young people had not been bullied at school but has been bullied by a pupil from school, and just over one in five had been bullied on their way to or from school. One-third has been bullied on social media, and one in ten had been bullied at home.
Compared to young people who were not LGBTQ+, young people who were LGBTQ+ were more likely to have been bullied at home (7% versus 17%), not at school but by a school pupil (22% versus 36%), and one the way to or from school (22% versus 36%).
Over three-quarters of the bullying was name-calling or teasing with six in ten subject to having lies or rumours spread about them, and over half were bullied about their appearance.
Males were statistically significantly more likely to have been pushed, hit, kicked or slapped compared to females (60% versus 35%) and have personal items damaged, taken or stolen (43% versus 20%).
Whilst young people who were white British were more likely to have been bullied in the last year compared to young people from minority ethnic groups (29% versus 23%), not surprisingly young people who were from minority ethnic groups were more likely to experience bullying related to racism (43% versus 8%) as did young people whose first language was not English compared to those whose first language was English (48% versus 11%). Young people whose first language was not English were more likely to be bullied “online, filmed and shared” compared to those whose first language was English (29% versus 11%).
Compared to young people who were not LGBTQ+, young people who were LGBTQ+ were more likely to have been bullied about their identity (21% versus 37%) or sexism (8% versus 24%) and also experience other forms of bullying (21% versus 37%).

There were relatively large differences in the percentages of young people who had been bullied in the last year among some specific groups. There was a statistically significant difference among males and females with 24% of males and 31% of females having been bullied in the last year. Young people whose daily activities were limited due to disabilities or long-term illness were more likely to have been bullied in the last year (44% versus 20%). As were young people who stated they were carers compared to non-carers (31% versus 22%), however, there were substantial differences in the percentage of young people who said they were carers with seven in ten young people in total saying they cared for others. It is unlikely that the percentages are as high as this, and the question is likely to have been misinterpreted. Younger pupils were more likely to state they were carers, and younger pupils were more likely to be bullied so it is likely that that age is a confounder, and that there might not be any difference in bullying between carers or non-carers. The percentage of young people who were LGBTQ+ was high at 46% and twice as high as young people who stated they were not LGBTQ+. This difference was statistically significant.
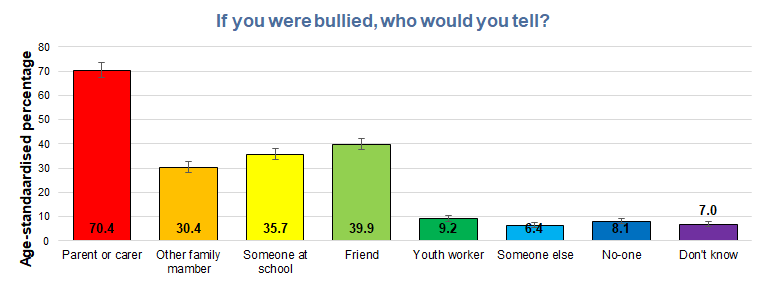
Overall, the majority would tell someone if they were bullied, although 8% stated they would tell no-one and a further 7% stated they didn’t know if they would tell anyone.
Males were statistically significantly more likely to say they would tell no-one compared to females (10% versus 4%) and also state that they didn’t know if they would tell anyone (11% versus 6%).
Young people from minority ethnic groups compared to young people who were white British were less likely to tell a parent or carer if they were bullied (64% versus 74%), as were young people whose first language was not English compared to those whose first language was English (57% versus 73%), and these young people were also less likely to tell another family member (24% versus 31%).
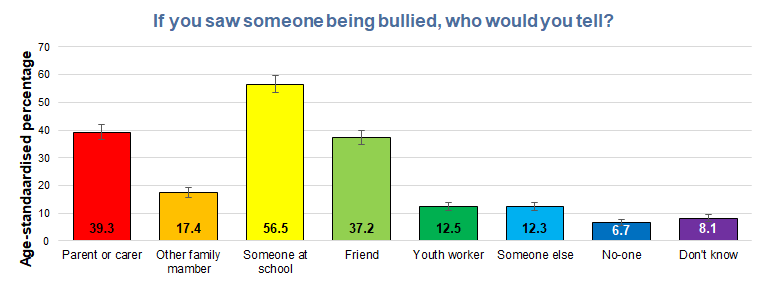
If they saw someone being bullied, just over half would tell someone from school, around four in ten would tell a parent or carer, and 37% would tell a friend.
Young people from minority ethnic groups compared to young people who were white British were less likely to tell a parent or carer if they had witnessed bullying (33% versus 42%), as were young people whose first language was not English compared to those whose first language was English (29% versus 41%).
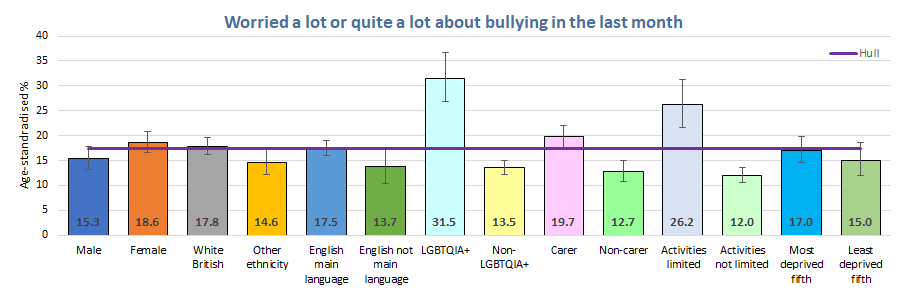
Overall, 17% had worried a lot or quite a lot about bullying in the last month, but this was much higher among young people who were LGBTQ+ with almost twice as many of them worrying about bullying (32%). Young people who whose activities were limited due to long-term illness or disability were also more likely to worry about bullying (26%) as were those who reported that they were carers (20%) although this is likely confounded with age as mentioned above as younger pupils were much more likely to worry a lot or quite a lot in relation to older pupils about virtually all of the life factors that the survey asked about.
Having an Adult to Talk to
Young people were asked if they had an adult to talk to if things were bothering them, and had the option of responding with yes, no, don’t know or rather not say.
In data analysis, it is common to exclude responses that are missing or uncertain, so if the percentages of stating they had someone to talk to is given out of the total number who answered yes or no, then over nine in ten young people had an adult to talk to if things were bothering them although the percentages were marginally lower for Year 11 males at 86%.
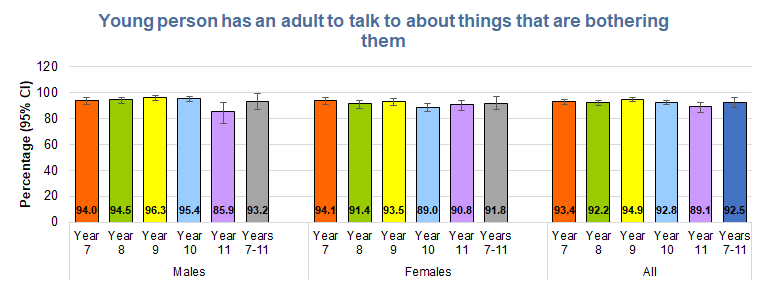
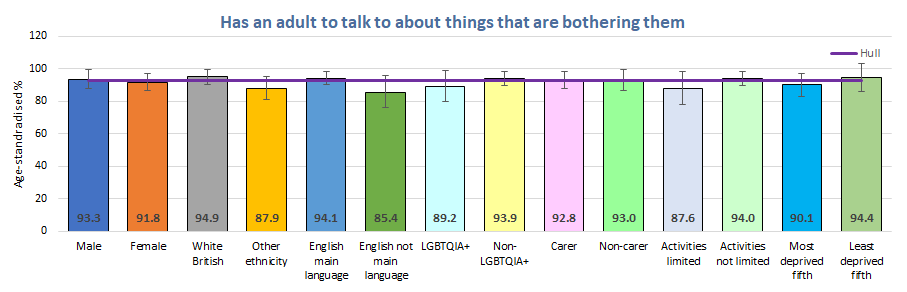
There were some slight differences between different groups of young people, but none of the differences were statistically significant.
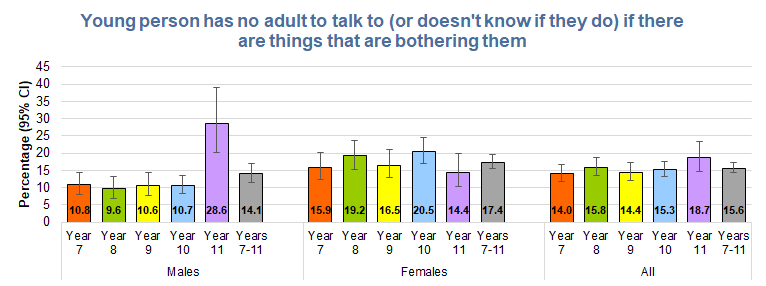
If the percentage who stated they did not have an adult to talk to or didn’t know was calculated the number who stated yes, no or don’t know, then around one in ten males in Years 7 to 10 and 29% of males in Year 11 did not have an adult to talk to or didn’t know. The percentages were higher among females around 15% for Years 7, 9 and 11, and around 20% for Years 8 and 10.
Feelings of Safety
Young people were asked how safe they felt at home, in their local area, at school, in the local park, in Hull city centre and online with responses very safe, fairly safe, a bit unsafe and very unsafe.
Over 95% of young people felt very safe or safe at home. Males tended to have higher percentages reporting feeling very safe at the different locations but as females tended to have the higher percentages reporting safe, and as a result, the percentages of young people who felt very safe or safe for males and females was relatively similar. Young people were the least likely to feel safe in the local park and in Hull city centre, although around three in ten did not feel safe at school.

Feelings of safety were consistently for both males and females for all school years with more than nine in ten feelings very safe or safe. Between 77% and 86% felt very safe at home.
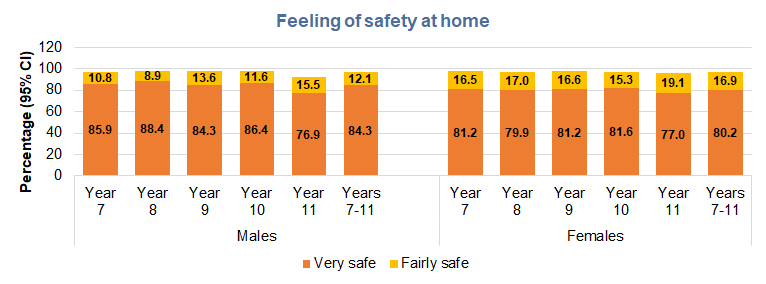
One in eleven young people who were LGBTQ+ felt very unsafe or a bit unsafe at home, and one in 16 young people who had daily activities limited due to long-term illness and disability.
Feelings of safety were also lower among people living in the most deprived fifth of areas of Hull compared to those living in the last deprived fifth of areas of Hull, although the differences were not statistically significant.
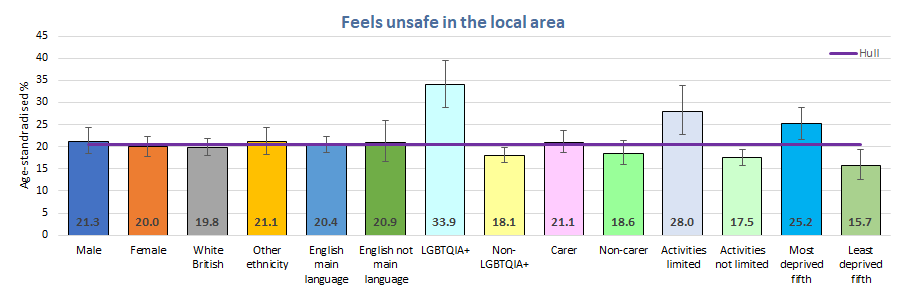
Around three-quarters of young people felt very safe or fairly safe in their local area. There were some variation across the school years and differences among males and females but they were not substantial. Males were more likely to feel very safe whereas females were more likely to report feeling fairly safe.

Young people who were LGBTQ+ and young people whose daily activities limited due to long-term illness and disability were also more likely to feel very unsafe or a bit unsafe in their local area. Just over one-third of young people who were LGBTQ+ felt unsafe. Feelings safety were also lower among people living in the most deprived fifth of areas of Hull compared to those living in the last deprived fifth of areas of Hull with 25% feeling unsafe in the more deprived areas of Hull compared to 16% in the less deprived areas of Hull.
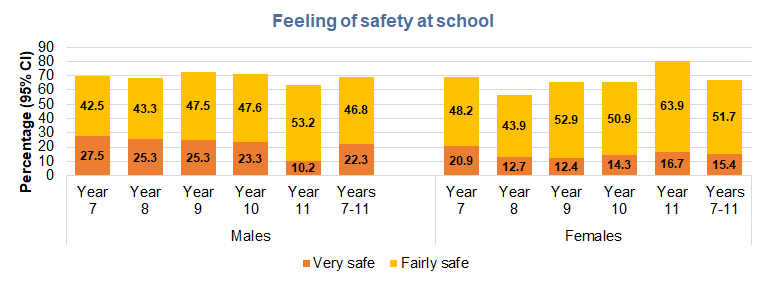
Seven in ten males (69%) and two-thirds (67%) of females felt very safe or fairly safe at school, although there were some differences across the school year groups. The percentages were lower among males in Year 11, and females in Year 8.
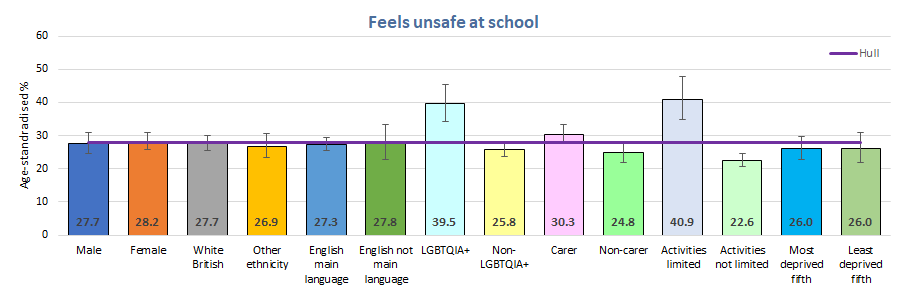
Four in ten young people who were LGBTQ+ and young people whose daily activities limited due to long-term illness and disability felt very unsafe or a bit unsafe at school.
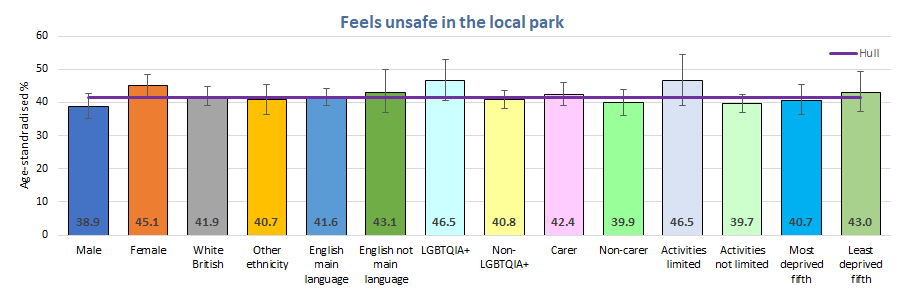
Feelings of safety in the local park were lower among females compared to males, and among Year 11 males. Almost six in ten males in Years 7 to 10 felt safe in their local park falling to 47% for Year 11 males (although as mentioned above the numbers surveyed were low for Year 11 males so the results need to be considered carefully).
Between 45% and 51% of females – depending on the school year – felt safe in the local park.

Females were more likely to feel unsafe in the local park (45%) compared to males (39%). There were slight differences between other groups of young people but none of these differences were statistically significant.
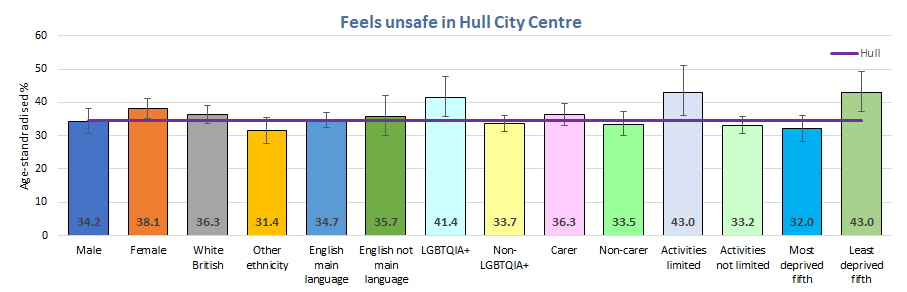
Around six in ten males in Years 7 to 10 felt safe in Hull city centre, and the percentage was lower at 42% among Year 11 males (although as previously mentioned there is more uncertainty associated with the percentages among Year 11 males).
Around half of females felt safe in Hull city centre, although the percentage was slightly lower among Year 8 females (46%) and higher among Year 11 females (65%).
It is likely that there will be differences in the frequency of going into Hull city centre for some of these different school years for males and females, and the ages at which they go alone or with friends into Hull city centre, rather than with adults, parents or carers.

Young people who were LGBTQ+ were more likely to feel unsafe in Hull city centre (41%) as were young people whose daily activities limited due to long-term illness and disability (43%) and young people living in the least deprived fifth of areas of Hull (43%).
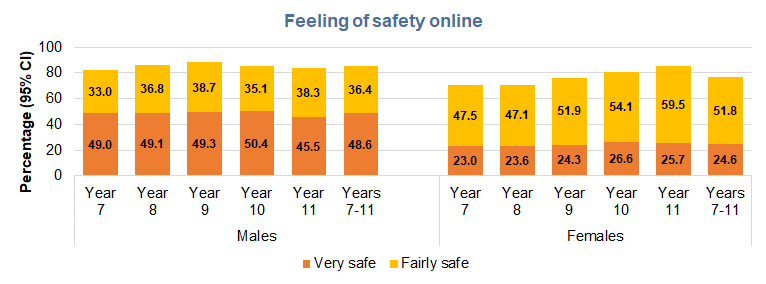
Over eight in ten males felt safe online, but feelings of safety whilst online were lower among females and lowest among younger females. The percentages increased from 71% among Year 7 females to 85% among Year 11 females.
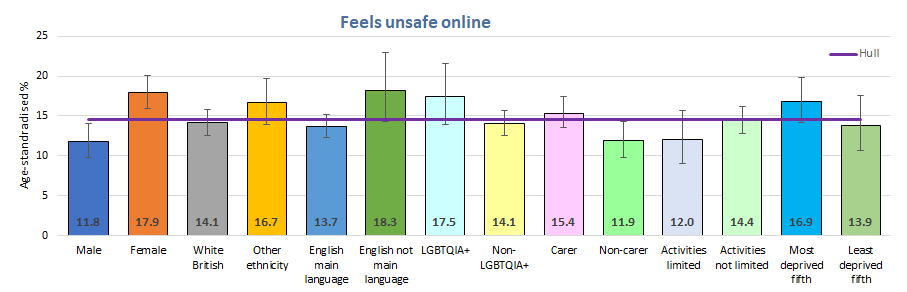
As mentioned above, feelings of safety were lower among females whilst being online. The difference in the percentages feeling unsafe whilst online was statistically significantly different among males (12%) and females (18%).
Mental Health of Children and Young People in England Survey 2023
Prevalence of Probable Mental Health Disorders and Trends Over Time
The State of the Nation 2021 and 2022 Children and Young People’s Wellbeing Research reports, as well as NHS Digital’s Mental Health of Children and Young People in England survey in 2017 and four subsequent waves of follow-up surveys in 2020, 2021, 2022 and 2023, estimated the prevalence of probable mental disorders among children in England.
The Strengths and Difficulties Questionnaire was used and includes 25 questions on different aspects of behaviour related to emotional problems, conduct problems, hyperactivity/inattention (restlessness), peer relationship problems and positive prosocial behaviour. The responses to the four problem scales can be viewed together to assess a person’s total difficulties, or separately to look at particular problems. The scores for these scales can then also be combined with answers to questions about the impact that the difficulties have on the child’s life to create a score which indicates likelihood of that child having a mental disorder from unlikely to probable.
Across England, one in nine (11.2%) of those aged 8 to 10 years had a probable mental health disorder in 2017, but this had increased to a 16.0% in 2020 and 17.7% in 2021 which could be partially due to the pandemic.. The percentages have since fallen slightly among 8-10 year olds to 15.7% in 2023.
However, the percentages estimated to have a probable mental health disorder has increased dramatically between 2017 and 2023 for England for both those aged 11-16 years and aged 17-19 years, as well as increasing sharply among those aged 20-25 years between 2021 and 2023.
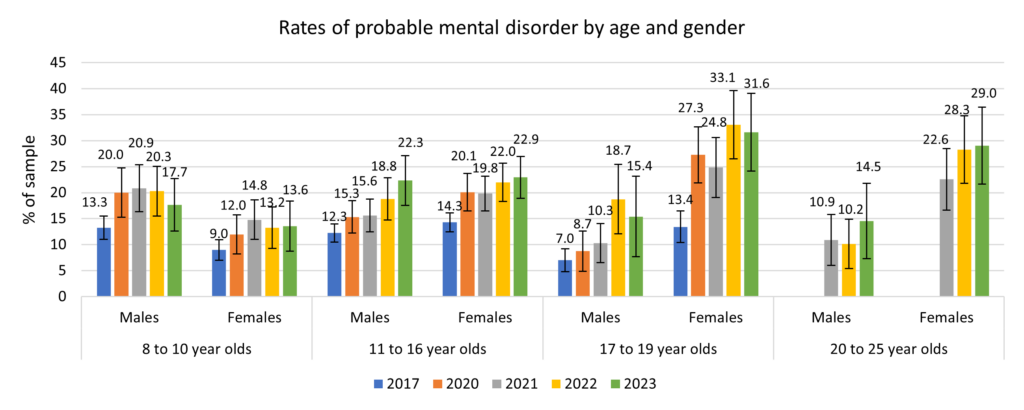
In England for 2023, compared to girls, boys were more likely to have a probable disorder (19.8% versus 20.8%) and possible disorder (10.8% versus 13.1%) among those aged 8-16 years, although the reverse was true for older ages with a much higher prevalence among females which was double that of males. Almost one-third (31.6%) of females aged 17-19 years were estimated to have a probable mental health disorder compared to 15.4% of males, and females were slightly more likely to have a possible mental health disorder (16.0% versus 14.7%). The percentages had increased substantially since 2017 when 13.4% of females and 7.0% of males were estimated to have a probable mental health disorder and 14.9% of females and 9.9% of males were estimated to have a possible mental health disorder.
The percentages among young adults did decrease slightly compared to young people aged 17-19 years. In 2023, it was estimated that 29.0% of females and 14.5% of males were estimated to have a probable mental health disorder and 13.0% of females and 15.8% of males were estimated to have a possible mental health disorder among those aged 20-23 years. This is also an increase since 2021 (data not available for 2017 for those aged 20-23 years) when 22.6% of females and 10.9% of males were estimated to have a probable mental health disorder and 13.3% of females and 12.1% of males were estimated to have a possible mental health disorder.
Applying Prevalence Estimates to Hull to Obtain Estimated Numbers in Hull
Based on the Office for National Statistics resident population estimates for 2024, there are 5,473 males and 5,136 females aged 8-10 years, 11,026 males and 20,697 females aged 11-16 years, 5,805 males and 5,121 females aged 17-19 years, and 10,664 males and 9,783 females aged 20-25 years. If the prevalence estimates above for England are applied to Hull’s population, it is possible to obtain the estimated number of children and young people in Hull with a probable or possible mental health disorder.
As mentioned below, in the Centre for Young Lives’ 2025 State of Childhood Vulnerability report, behind every number is a child who needs support – often facing multiple, overlapping challenges that can be rooted in poverty, instability, and inequality.
Children who are at most of need and who are most vulnerable are more likely to live in relative poverty, and due to the much higher levels of deprivation within Hull compared to England, the estimated numbers of children and young people impacted by mental health disorders is likely to be higher than stated.
| Sex | Mental health disorder | Aged 8-10 | Aged 11-16 | Aged 8-16 | Aged 17-19 | Aged 20-25 |
| All | Unlikely | 7,658 | 14,211 | 21,897 | 6,742 | 12,893 |
| Possible | 1,288 | 2,598 | 3,880 | 1,672 | 3,150 | |
| Probable | 1,663 | 4,914 | 6,555 | 2,515 | 4,405 | |
| Male | Unlikely | 3,596 | 7,312 | 10,908 | 4,060 | 7,472 |
| Possible | 910 | 1,253 | 2,167 | 851 | 1,761 | |
| Probable | 967 | 2,461 | 3,424 | 894 | 1,431 | |
| Female | Unlikely | 4,062 | 6,899 | 10,989 | 2,682 | 5,421 |
| Possible | 378 | 1,345 | 1,713 | 821 | 1,389 | |
| Probable | 696 | 2,453 | 3,131 | 1,618 | 2,974 |
Self-Harm and Ability to Feel They Can Be Themselves and Safe at School
Rates of self-harm and talk of self-harming was much higher among young people who had a probable mental health disorder, and school absence was substantially greater. Young people who had a probable mental health disorder were more likely to feel that they could not be themselves at school, less likely to feel safe at school and less likely to enjoy learning. They were also less likely to have at least one friend they could turn to for support.
Knowledge and Trust of Services and Access to Support
Over half had accessed mental health and wellbeing support at school. The majority did know they could get help for worries and mental health concerns (just over 80%), agreed that they felt comfortable talking to adults at their school about mental health (around six in ten), agreed that they could get mental health support at school without others finding out (two-thirds), agreed that support from school was helpful (just under two-thirds), and agreed they could access support from school when they needed it (three-quarters).
Among 8-16 year olds, 85% had sought help and advice for a mental health concern among those who had a probably mental health disorder (74% for those with a possible disorder and 64% of those who were unlikely to have a disorder). Among 8-16 year olds with a probable mental health disorder, almost three-quarters (74%) accessed support through education, 49% through health, 42% obtained support from family or friends and 35% accessed online support. Among 17-24 year olds, 63% had sought help and advice for a mental health concern among those who had a probably mental health disorder (60% for those with a possible disorder and 43% of those who were unlikely to have a disorder). Among 17-24 year olds with a probable mental health disorder, two-thirds (66%) obtained support from family or friends, 45% through health, 43% accessed online support, and 21% through education.
Impact or Consequence of Life Factors on Mental Wellbeing
Among 8-16 year olds, compared to children and young people unlikely to have a mental health disorder, children with a probable mental health disorder were more likely to have had a parent or partner who lost their job or business (2.9% versus 6.6%), have had a reduction in household income (12.6% versus 22.3%), fallen behind will bills, rent or mortgage (6.8% versus 18.7%), could not afford to buy enough food or had to use a food bank (3.5% versus 15.3%), could not afford to keep their home warm enough (7.6% versus 19.9%), have lost their home or became homeless (0.2% versus 0.9%) and had a parent or somebody close to them is or was seriously ill (10.6% versus 13.7%). Children and young people aged 8-16 years with a probable mental health disorder were more likely to have had at least one of these factors present (41.7%) compared to children and young people unlikely to have a mental health disorder (29.5%), and as a consequently less likely to have none of the above (58.3% versus 70.5%).
Among young people aged 17-24 years, compared to those unlikely to have a mental health disorder, those with a probable mental health disorder were more likely have moved in with a partner (5.8% versus 10.7%), moved out of their parents or carer’s home (9.9% versus 14.8%), lost their job or business (3.6% versus 11.2%), had a baby (1.0% versus 1.3%), lost their home or become homeless (0.8% versus 6.5%), had a reduction in household income (8.1% versus 15.4%), fallen behind will bills, rent or mortgage (5.4% versus 20.6%), could not afford to buy enough food or had to use a food bank (4.2% versus 13.6%), could not afford to keep their home warm enough (8.8% versus 18.8%), being ill or had somebody close to them is or was seriously ill (10.4% versus 19.9%). Young people with a probable mental health disorder were less likely to have started a new job or course of study compared to those unlikely to have a disorder (30.2% versus 39.2%). Young people aged 17-24 years with a probable mental health disorder were more likely to have had at least one of these factors present (67.1%) compared to young people unlikely to have a mental health disorder (55.5%), and as a consequently less likely to have none of the above (32.9% versus 44.5%).
Among children and young people aged 8-16 years, parents were much more likely to agree that they feel worried about money among parents of those with a probable mental health disorder compared to those unlikely to have a disorder (57.2% versus 39.0%), and they were less likely to agree that they could afford to give their child a healthy diet (80.4% versus 90.2%), afford the right clothes, shoes and equipment for school or college (73.1% versus 89.0%), afford their child to take part in activities outside school such as family days out, swimming or other hobbies (61.1% versus 79.8%) and afford or have access to transport to take their child where they needed to go (75.3% versus 91.1%).
The financial impact was also felt by the child. Among those aged 11-16 years, one fifth (21.0%) agreed that their family struggle more than other families to afford the things that they need among young people with a probable mental health disorder compared to one fifth (10.3%) of those unlikely to have a disorder. There was also fewer young people with a probable mental health disorder compared to those unlikely to have a disorder agreeing that their family could afford to keep their home warm enough (79.4% versus 89.2%), have enough food for them to eat, eat a healthy diet including fruit and vegetables (89.5% versus 96.1%), afford to do activities and fun things together as a family (72.7% versus 84.5%), and afford to buy them the right clothes and shoes for school (83.4% versus 96.3%). Among young people aged 17-25 years, there was also an increased level of concern around their financial situation among young people with a probable mental health disorder compared to those unlikely to have a disorder with higher percentages agreeing that they worry about money (69.4% versus 40.2%), and lower percentages agreeing that they could afford healthy food (60.9% versus 88.7%), afford for me to have the clothes, shoes or equipment needed for daily life (69.4% versus 91.1%), afford to take part in activities such as sport, days out or socialising with friends (51.9% versus 84.0%), and afford to access transport to do the things needed in daily life (70.0% versus 92.4%).
Young people with a probable mental health disorder compared to those unlikely to have a disorder were more likely to have been bullied online (19.3% versus 5.9% among 11-16 year olds and 26.1% versus 7.6% among 17-24 year olds) and less likely to feel safe online (55.8% versus 64.6% among 11-16 year olds and 42.8% versus 65.4% among 17-24 year olds). Young people aged 11-16 years with probable mental health disorder compared to those unlikely to have a disorder were more likely to have been bullied i the last year in person (36.9% versus 7.6%) and online (10.8% versus 2.6%).
Among young people aged 17-23 years, those with probable mental health disorder compared to those unlikely to have a disorder were less likely to feel very or quite optimistic about their future in terms of job prospects (30.9% versus 70.2%), having enough money (21.5% versus 61.1%), having somewhere secure to live (42.2% versus 76.9%), their health including mental health and wellbeing (24.2% versus 78.0%), their family’s health (42.3% versus 75.9%), the environment (13.4% versus 34.7%), Brexit (5.0% versus 11.2%), COVID-19 (27.0% versus 48.9%), relationships with friends (53.5% versus 87.7%), and relationships with family (70.0% versus 92.0%).
Eating Disorders
Within the Mental Health of Children and Young People in England 2023, screening was also undertaken for possible eating problems. The prevalence estimates were 9.8% for males and 14.9% for females among 11-16 year olds, 42.3% for males and 77.5% for females among 17-19 year olds, and 43.0% for males and 72.3% for females among 20-25 year olds. They report that the prevalence estimates have increased substantially since 2017 although some of the increase could be due to better awareness and recording.
Among those aged 11-16 years, it was estimated that 0.0% of males and 0.4% of females had anorexia nervosa, 0.2% of males and 0.8% of females had bulimia nervosa, and 0.6% of males and 2.9% of females had other eating disorders, and overall that 1.0% of males and 4.3% of females had any eating disorder.
Among those aged 17-19 years, it was estimated that 0.6% of males and 6.4% of females had anorexia nervosa, 0.0% of males and 3.6% of females had bulimia nervosa, and 4.5% of males and 11.5% of females had other eating disorders, and overall that 5.1% of males and 20.8% of females had any eating disorder.
Among those aged 20-25 years, it was estimated that 0.0% of males and 0.6% of females had anorexia nervosa, 1.9% of males and 1.6% of females had bulimia nervosa, and 1.6% of males and 6.9% of females had other eating disorders, and overall that 3.6% of males and 8.5% of females had any eating disorder.
Based on the Office for National Statistics resident population estimates for 2024, there are 11,026 males and 20,697 females aged 11-16 years, 5,805 males and 5,121 females aged 17-19 years, and 10,664 males and 9,783 females aged 20-25 years. If the prevalence estimates above for England are applied to Hull’s population, it is possible to obtain the estimated number of children and young people in Hull with an eating disorder. It is possible figures are higher in Hull as it is likely that increased mental health needs, poverty, vulnerability and levels of child obesity increase the risk.
| Sex | Eating disorder | Aged 11-16 | Aged 17-19 | Aged 20-25 |
| All | Anorexia nervosa | 44 | 362 | 64 |
| Bulimia nervosa | 111 | 185 | 365 | |
| Other eating disorder | 394 | 850 | 851 | |
| Any eating disorder | 564 | 1,364 | 1,215 | |
| Male | Anorexia nervosa | 0 | 33 | 0 |
| Bulimia nervosa | 24 | 0 | 207 | |
| Other eating disorder | 81 | 263 | 175 | |
| Any eating disorder | 105 | 267 | 382 | |
| Female | Anorexia nervosa | 44 | 329 | 64 |
| Bulimia nervosa | 87 | 185 | 158 | |
| Other eating disorder | 313 | 587 | 676 | |
| Any eating disorder | 459 | 1,067 | 833 |
National Estimates of Poor Mental Health Applied to Hull
Nationally, the numbers of young people aged 15 year with mental health issues has been estimated for a classroom of 30 pupils.
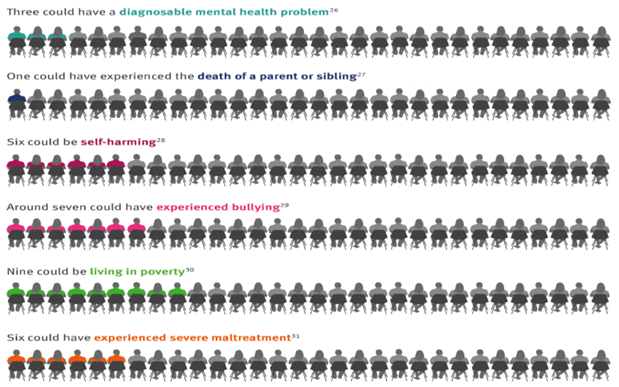
The most common disorder in early years and primary school are behavioural disorders and the most common in secondary school and post 16 establishments are emotional disorders. Early intervention is key to reducing this prevalence.
Prevalence is increasing both nationally and locally. There are also marked gender differences, for instance, older girls are more likely to experience emotional disorders.
The prevalence of mental ill health is higher amongst vulnerable groups of children and young people:
- LGBT+ young people are more likely to have a diagnosable mental health problem (34.9% compared to 13.2%).
- Mental health problems are more common in children living in lower income households (9.0% compared to 4.1%).
- Children living with a parent with poor mental health are the most at risk group.
- Over a third of 5 to 19 year olds with a mental health problem (35.6%) were also recognised as having special educational needs.
- School exclusions are more common in children with a mental health difficulty (6.8%) than those without (0.5%).
- Other risk factors include poor housing, being in or leaving care, being a young carer or experiencing bereavement.
Looked After Children
Just under half of looked after children in Hull had levels of emotional wellbeing which was a cause for concern in 2023/24 which was higher than England and the region.
This relates to children aged 5-16 years at the date of their latest assessment who have been in care for at least 12 months on the 31 March of the year whose strengths and difficulties questionnaire (SDQ) score is 17 or more.
Compared with benchmark
| Indicator | Period | England | Yorkshire and the Humber region (statistical) | Kingston upon Hull | East Riding of Yorkshire | North East Lincolnshire | North Lincolnshire | York | North Yorkshire UA | Barnsley | Doncaster | Rotherham | Sheffield | Bradford | Calderdale | Kirklees | Leeds | Wakefield |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
Percentage of looked after children whose emotional wellbeing is a cause for concern (Persons 5-16 yrs) | 2024/25 | 42.0 | 45.0 | 53.0 | 50.0 | 45.0 | 47.0 | 45.0 | 50.0 | 56.0 | 43.0 | 44.0 | 52.0 | 31.0 | 46.0 | 46.0 | 42.0 | 49.0 |
| Indicator | Period | England | Yorkshire and the Humber region (statistical) | Kingston upon Hull | East Riding of Yorkshire | North East Lincolnshire | North Lincolnshire | York | North Yorkshire UA | Barnsley | Doncaster | Rotherham | Sheffield | Bradford | Calderdale | Kirklees | Leeds | Wakefield |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
Percentage of looked after children whose emotional wellbeing is a cause for concern (Persons 5-16 yrs) | 2024/25 | 42.0 | 45.0 | 53.0 | 50.0 | 45.0 | 47.0 | 45.0 | 50.0 | 56.0 | 43.0 | 44.0 | 52.0 | 31.0 | 46.0 | 46.0 | 42.0 | 49.0 |
There has been some year-on-year variation in the percentage of looked after children whose emotional wellbeing is a cause for concern, but for most years there has been no statistically significant difference in the percentage between Hull and England (except for 2018/19 when the percentage in Hull was significantly lower than England). However, in the last year the percentage has increased in Hull and for 2023/24, the percentage is statistically significantly higher than England.
Compared with benchmark
Percentage of looked after children whose emotional wellbeing is a cause for concern (Persons 5-16 yrs)
|
Period
|
Kingston upon Hull |
Yorkshire and the Humber region (statistical)
|
England
|
||||
|---|---|---|---|---|---|---|---|
|
Count
|
Value
|
95%
Lower CI |
95%
Upper CI |
||||
| 2015/16 | • | 39 | 39.0% | 30.0% | 48.8% | 39.1% | 37.8% |
| 2016/17 | • | 40 | 41.7% | 32.3% | 51.7% | 42.8% | 38.1% |
| 2017/18 | • | 41 | 46.1% | 36.1% | 56.4% | 42.7% | 38.6% |
| 2018/19 | • | 74 | 28.0% | 22.5% | 33.1% | 41.0% | 39.0% |
| 2019/20 | • | 134 | 38.0% | 33.2% | 43.2% | 40.0% | 38.0% |
| 2020/21 | • | 135 | 34.0% | 29.1% | 38.3% | 39.0% | 37.0% |
| 2021/22 | • | 140 | 34.0% | 29.6% | 38.7% | 39.0% | 37.0% |
| 2022/23 | • | 139 | 42.0% | 36.7% | 47.2% | 43.0% | 40.0% |
| 2023/24 | • | 188 | 48.0% | 43.2% | 53.0% | 42.0% | 41.0% |
| 2024/25 | • | 196 | 53.0% | 47.6% | 57.7% | 45.0% | 42.0% |
Source: Department for Education
Presenting Issues for Local Young People
The main presenting issues for young people accessing Hull’s Targeted Early Help / Getting Help programme were as follows:
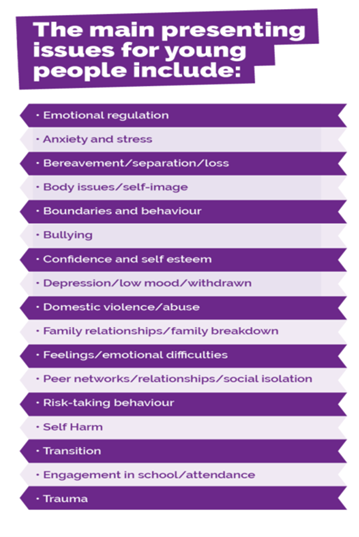

The main presenting issues for parents were as follows:

Worsening Levels of Vulnerability Among Young People in England Following the Pandemic
The Centre for Young Lives’ 2025 State of Childhood Vulnerability report, which was published in July 2025, warns that the COVID-19 pandemic is still casting a long shadow over millions of children in England five years on.
They state that many measures of vulnerability such as poverty, children’s mental health, Special Educational Needs, school attendance, and the number of children going into social care have worsened and continued to hold children back since the pandemic. The report shows how since the pandemic more children are living in poverty and temporary accommodation, how school absence, exclusion0s and home education have rocketed, and how the number of children with Special Educational Needs continues to soar, how many more children are being taking into care, and how many more children and young people are struggling with a diagnosable mental health problem.
They summarise some of the statistics for England (some of the changes could be due – at least in part – to increased awareness, recognition and recording of information):
- One-third of children in the UK are living in relative poverty in the UK for 2023/24 (the figure is higher in Hull).
- There has been an increase of one-third in the number of children living in temporary accommodation between 2018/19 and 2023/24.
- The percentage of children who are persistently absent from school has almost doubled from 2018/19 to 2023/24.
- Almost 50,000 children were in alternative provision in 2024/25 which is an increase of 82% since 2018/19.
- At least 153,3000 children were electively home educated in 2023/24 an increase of almost one-third since 2021/22.
- Almost one million young people aged 16-24 years were not in education, employment or training in the UK between January and March 2025 which is an increase of 19% since January and March 2019.
- The number of children who were looked after has increased between 2018 and 2024 by 11% with a doubling among young people aged 16+ years entering the care system between 2013 and 2023.
- Almost one-third of adults where domestic abuse is reported had children aged under 16 years present in the household in 2023 which is an increase of 30% since 2017/18.
- There has been an increase of one-third in the number of children with Special Educational Needs between 2017/18 and 2023/24.
- There has been a 90% increase in the children who have an Education, Health and Care Plan between 2017/18 and 2023/24.
- The number of children identified as autistic has more than doubled between 2017/18 and 2024/25.
- One in five children and young people aged 8-16 years had a diagnosable mental health condition in 2023 which has increased from one in ten in 2017.
- Child criminal exploitation was identified in 15,600 children in need assessments in 2024 which is an increase of over 50% since 2022.
- One in five 13-17 year olds have been a victim of violence in 2024 which has increased from 14% in 2022.
The report argues that taken together, these indicators reveal a generation of post-COVID children facing vulnerabilities that threaten to shape their futures long into adulthood. Behind every number is a child who needs support – often facing multiple, overlapping challenges that can be rooted in poverty, instability, and inequality. The report also notes that there are many children that the data does not capture. Some of the most vulnerable children are continuing to slip under the radar entirely. Not only do they not appear in the data, but often they are not receiving any support at all.
From the Health Foundation’s report into children and young people’s mental health and ‘COVID-19 and the road ahead’, they state that mental health conditions have become more common since the start of the pandemic. They estimate that between 2017 and 2021, the percentage of 6 to 16 year olds with a probable mental health conditi0n increased from one in nine (11.6%) to one in six (17.4%). They recognise that increased awareness and recognition of mental health conditions in children and young people may have contributed to the increase, but they indicate that the prevalence of mental heath conditions is likely increasing. Girls aged 17-19 years had the highest increases in prevalence almost doubling from one in seven (13.4%) in 2017 to one in four (24.8%) in 2021, but boys of the same age showed no statistically significant change over time. In 2021, children and adolescents with a probable mental health condition were twice as likely to live in households newly falling behind on bills (12.8%, compared with 6.7% of 6 to 16-year-olds without a mental health condition).
Societal changes in the last few years in relation to social media is considered to adversely affect children and young people’s mental health and emotional wellbeing.
Their report also details the referrals into Children and Young People Mental Health Services (CYPMHS) for England. They state that the rate of new referrals to CYPMHS initially slowed after March 2020, when schools closed due to COVID-19 restrictions and families had to navigate changes in access to primary care. In April 2020, a month after the first lockdown started in England, new referrals were 35% lower than a year before and they did not recover to previous levels until July 2020. After this point, they rapidly accelerated and subsequently reached a record high of 100,000 new referrals per month in May 2021. They state that the data show encouraging signs that CYPMHS capacity has also expanded to treat an increasing number of children and young people, as shown by the number of first-time appointments for those younger than 18. In 2020, during the first COVID-19 wave, the number of first contacts initially slowed but later recovered to previous levels. In 2021, based on data from January to September, there were on average over 55,000 first contacts per month, an increase of 17% compared with the same period in 2020. According to NHS Digital monthly mental health statistics, over 340,000 children and young people were in contact with CYPMHS in July 2021, meaning they were waiting to commence treatment or currently receiving treatment – the highest number ever recorded. Comparing the period between January and September, the number of people in contact with CYPMHS was 24% higher in 2021 than in 2020, and 44% higher than in 2019. This increase is partly related to changes in reporting, with the number of providers submitting data increasing over time. They state that changes in reporting methodology have created additional challenges in determining the extent to which the CYPMHS caseload has increased.
Self-Harm
Information relating to self-harm among young people aged 10-24 years is presented under Suicide and Self-Harm within Adults.
Strategic Need and Service Provision
In order to improve mental health and wellbeing, WHO state that it is necessary to have an environment that supports mental health. National mental health policies should be concerned both with mental disorders and, with broader issues that promote mental health. Mental health promotion should be mainstreamed into governmental and nongovernmental policies and programmes. In addition to the health sector, it is essential to involve the education, labour, justice, transport, environment, housing, and welfare sectors.
Both adults and children with general mental health issues need to be identified early and encouraged to seek help early so that the consequences in terms of the effects on family, education and employment are minimised, and issues are not escalated so to reduce the need for crisis and/or medical interventions. It should be recognised that specific groups of people may be more likely to have mental health issues due to their circumstances, such as poverty, asylum seekers, social isolation. There is a need to improve and expand early help and targeted interventions to improve young people’s emotional health and wellbeing and build resilience to enable them to cope with challenging life events.
In 2018 NHS England set out its ten year long term plan for the priorities to be delivered for children and young people.
- Additional investment in community based mental health services.
- The creation of mental health support teams in schools and colleges.
- Safe places and crisis cafés open 24/7 to support young people.
- Home Intensive Treatment teams to support young people in their own home and the community to reduce the need for in patient beds.
- Additional investment into community eating disorder services and prevention and promotion offers.
Prevention and early intervention relating to children and young people in terms of the Thriving, Getting Advice and some aspects of Getting Help, encompass only part of the whole mental health system for Hull. More information on mental health and emotional wellbeing and early intervention is also available under Early Help and Prevention under Child Development within Children and Young People.
Hull has adopted the THRIVE Framework to describe and organise system efforts in relation to children and young people’s emotional and mental health. For more information on the Thrive Framework and an up-to-date list of services available to support children and young people’s emotional and mental health, mapped against the THRIVE model in Hull, please visit: https://www.howareyoufeeling.org.uk
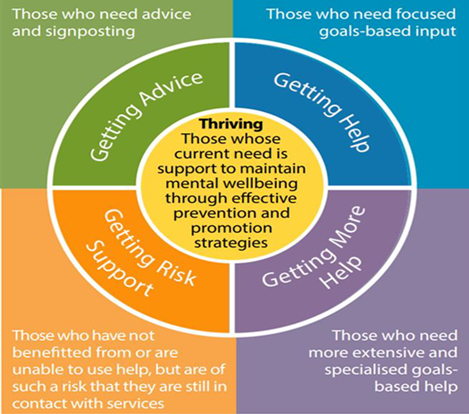
It is recognised the mental and emotional wellbeing has been detrimentally affected for many children and young people due to COVID-19 and lockdowns. Furthermore, the effect has not been felt evenly across society and the most vulnerable have generally been affected the worst, increasing the inequalities gap. Recognition is not sufficient and increased resources need to be made available to improve mental health and emotional wellbeing in children and young people.
A Mentally Healthy Hull strategy has been produced which looks at how, as a city, we can collectively boost good mental health and prevent and reduce the impact of mental health problems.
Resources
National Institute for Health and Care Excellence, Social and emotional wellbeing for children and young people: Local government briefing. www.nice.org.uk. 2013, National Institute for Health and Care Excellence: London.
World Health Organization. Mental health: strengthening our response: https://www.who.int/news-room/fact-sheets/detail/mental-health-strengthening-our-response
WHO Special Initiative for Mental Health (2019-2023): Universal Health Coverage for Mental Health. World Health Organisation, 2019. https://apps.who.int/iris/handle/10665/310981
Hull’s Young People Health and Wellbeing Survey
Mental Health of Children and Young People in England, 2017. Official statistics, survey. NHS Digital, November 2018.
Mental Health of Children and Young People in England, 2017 [PAS] – NDRS (digital.nhs.uk)
Mental Health of Children and Young People in England, 2023 – wave 4 follow up to the 2017 survey. https://digital.nhs.uk/data-and-information/publications/statistical/mental-health-of-children-and-young-people-in-england/2023-wave-4-follow-up
State of the Nation 2021: Children and Young People’s Wellbeing. Research report. Department for Education, February 2022. https://www.gov.uk/government/publications/state-of-the-nation-2021-children-and-young-peoples-wellbeing
State of the Nation 2022: Children and Young People’s Wellbeing. Research report. Department for Education, February 2023. https://www.gov.uk/government/publications/state-of-the-nation-2022-children-and-young-peoples-wellbeing
Strengths and Difficulties Questionnaire. https://www.sdqinfo.org/
The Health Foundation. Children and young people’s mental health. COVID-19 and the road ahead. https://www.health.org.uk/news-and-comment/charts-and-infographics/children-and-young-people-s-mental-health
NHS Digital. Mental Health Services Monthly Statistics. https://digital.nhs.uk/data-and-information/publications/statistical/mental-health-services-monthly-statistics
THRIVE Framework. https://www.annafreud.org/mental-health-professionals/thrive-framework/
How are you feeling today? THRIVE Hull. https://www.howareyoufeeling.org.uk/
Centre for Young Lives. Centre for Young Lives’ 2025 State of Childhood Vulnerability report warns the Covid pandemic is still casting a long shadow over millions of children in England five years on | Centre for Young Lives | Press Release, July 2025.
Updates
This page was last updated / checked on 21 April 2026.
This page is due to be updated / checked in September 2026.