Index
This topic area covers statistics and information relating to epilepsy in Hull including local strategic need and service provision.
This page contains information from the Office for Health Improvement & Disparities’ Fingertips. Information is taken ‘live’ from the site so uses the latest available data from Fingertips and displays it on this page. As a result, some comments on this page may relate to an earlier period of time until this page is next updated (see review dates at the end of this page).
Headlines
- For 2024/25, there are 2,608 patients aged 18+ years diagnosed with epilepsy among patients registered with Hull GPs. This represents 1.0% of registered patients aged 18+ years which is higher than England (0.8%).
- There was an association between diagnosed prevalence of epilepsy and deprivation. Practices serving the patients living in the most deprived areas of Hull had a significantly higher prevalence of diagnosed epilepsy compared to practices serving patients living in the least deprived areas of Hull.
- There were 70 hospital admissions for epilepsy among under 19s in Hull for 2023/24 which was 37% higher than England (109 versus 79 admissions per 100,000 population). The admission rate in Hull has decreased over time although there is year-on-year variability due to the relatively small number of admissions, and it is possible that some people may have been admitted more than once in the year.
- Over the five year period 2020/21 to 2024/25, there were 1,420 admissions to Hull residents where the primary cause of the admission was epilepsy with around 300 admissions each year (slightly fewer in 2020/21 likely associated with the COVID-19 pandemic). More admissions were among males compared to females (775 versus 645). Admissions were highest among children and people aged 75+ years. However, there were a number of patients that were admitted more than once during the five year period. The 1,420 admissions were from 755 patients with two-thirds having a single admission (490; 65%) and 135 (18%) admitted twice, 60 (7.9%) admitted three times, 20 (2.6%) admitted four times, 20 (2.6%) admitted five times, and 30 (4.0%) admitted on six or more occasions in the five year period.
- There were 35 deaths registered over the five year period 2021 to 2025 among Hull residents where the underlying cause of death was epilepsy. Six in ten of these deaths were among men, and men had a younger average age of death compared to women (52.2 years versus 71.1 years). Among men, there were eight deaths among men aged 20-39 years, four deaths among men aged 40-59 years, seven deaths among men aged 60-79 years and two deaths among men aged 80+ years. Among women, there were four deaths among women aged under 60 years, three deaths among women aged 60-79 years and seven deaths among women aged 80+ years.
The Population Affected – Why Is It Important?
Epilepsy is a condition that affects the brain and causes seizures (sometimes called fits). It cannot currently be cured, but treatment can often help manage it.
Epilepsy happens when the normal electrical activity in your brain changes. It’s thought that epilepsy is often related to the genes you inherit from parents, or to changes in your genes. It’s sometimes caused by damage to the brain, for example after a head injury, a stroke or an infection. But for many people it’s not clear what causes it.
From the NHS, usually the only symptom of epilepsy is having seizures, and symptoms of seizures can include:
- the body becoming stiff or floppy
- suddenly falling to the floor
- jerking or twitching movements of the body
- peeing unintentionally
- losing awareness of what’s around which could also include staring into space and not being able to respond normally
- unusual feelings or sensations, such as strange smells, numbness or tingling, changes in your vision, or suddenly feeling scared
- unusual behaviour, such as fidgeting or walking around, and a person not being aware of what they are doing
A seizure usually lasts a few seconds or minutes, and stops by itself. Some people might be aware of having a seizure and remember it afterwards, but others may not. Symptoms of epilepsy often start in young children and people over 50, but it can happen at any age.
Someone having a seizure should be treated as an emergency if it is the first time it has happened, it lasts longer than is usual for them (or longer than five minutes if it is unknown how long their seizures normally last for), they do not recover as usual afterwards or have another seizure without recovering between seizures, or a person has three or more seizures in 24 hours. An ambulance should also be called if the person does not regain full consciousness, is seriously injured during the seizure or has difficulty breathing after the seizure.
People with epilepsy do not always need to go to hospital when they have a seizure. They usually have a care plan that states what should be done.
Having a seizure does not always mean a person has epilepsy, as seizures can have other causes. People will usually be diagnosed with epilepsy if they’ve had more than one seizure or if tests show that they are at a risk of having more seizures.
There are different types of epileptic seizure. They can affect people differently, and people can have just one type of seizure or more than one different type. The main types of epileptic seizure are:
- tonic clonic seizures, where you become unconscious and may fall, your muscles get stiff and your body jerks and shakes
- tonic seizures, where your muscles suddenly get stiff and you may fall, then recover quickly
- atonic seizures, where your muscles suddenly go floppy and you may fall, then recover quickly
- absence seizures, where you briefly lose awareness of what’s going on around you
- focal seizures, where you have unusual feelings, sensations or movements
- myoclonic seizures, where your muscles briefly jerk
People who have epilepsy are supported by their GP and a team of specialists, and will have a check up at least once a year. A care plan will be put in place.
The main treatment for epilepsy is medicine to prevent seizures, called anti-epileptic or anti-seizure medicine. There are other medicines that can be used as emergency treatment given by a family member or carer, if a seizure that lasts longer than usual. There are different anti-epileptic medicines, and the medicine recommended will depend on the type of seizures, age, sex and if the person has other conditions.
Epilepsy affects everyone differently. It can be a life-long condition, or it can get better. How it affects you depends on the type of seizures you have, how often they happen and how well your treatment works.
For most people, medicine works well to prevent or reduce seizures, and epilepsy has a small impact on their daily life. But some people have seizures that are harder to control, and need more support.
Seizures are not usually harmful, although they can cause accidents or injuries. The risk of seizures may affect the type of work or activities you can do, and you may need to take extra safety measures.
An epileptic seizure usually stops by itself and does not cause any lasting problems. Rarely, a seizure can last a long time, or you may have several seizures without recovering in between. This is called status epilepticus, and needs urgent treatment to prevent damage to your brain. There’s also a small risk of dying suddenly, called sudden unexpected death in epilepsy (SUDEP). But this is rare, and epilepsy treatment can reduce the risk.
There are implication on pregnancy too. If a partner takes epilepsy medicine, they may need to change their medicine as some some epilepsy medicines can affect sperm, which could harm a baby. If a women has epilepsy, they may also need to change their medication, and there is a chance they’ll have more seizures during pregnancy. They may need extra maternity and others appointment and tests.
There is advice for people when they are with someone having a seizure:
- only move them if they’re in danger, such as near a busy road or hot cooker
- cushion their head if they’re on the ground
- loosen any tight clothing around their neck, such as a collar or tie, to aid breathing
- turn them on to their side after their convulsions stop in a recovery position.
- stay with them and talk to them calmly until they recover
- note the time the seizure starts and finishes
If the person is in a wheelchair, put the brakes on and leave any seatbelt or harness on. Support them gently and cushion their head, but do not try to move them.
Nothing should be put in their mouths, and they should not have any food or drink until they have fully recovered.
The Hull Picture
Prevalence
The Office for Health Improvement & Disparities’ Fingertips gives the percentage of patients registered with Hull GPs who are diagnosed with epilepsy. The sub Integrated Care Board areas which include Hull are within the Humber and North Yorkshire Integrated Care Board. In Fingertips, the sub-ICB area referenced by 03F relates to Hull (see Integrated Care Board for the codes relating to the other local sub-ICB areas).
For 2024/25, the prevalence of epilepsy among patients registered with Hull GPs at 1.0% which is comparable to most other areas within the Humber and North Yorkshire Integrated Care Board, but higher than England (0.86%).
However, there is only one point out of 635 points in total for practices for 2024/25 for “the contractor establishes and maintains a register of patients aged 18 or over receiving drug treatment for epilepsy”. With a relatively low number of points (and thus financial incentive as each point has a financial reward) assigned to epilepsy and no further indicators relating to ongoing care, it is likely that epilepsy is under-reported on the GP systems (see Local Analysis of Quality and Outcomes Framework Data for more information).
Compared with benchmark
| Indicator | Period | England | NHS Humber and North Yorkshire Integrated Care Board - QOQ | Humber and North Yorkshire ICB - 02Y | Humber and North Yorkshire ICB - 03F | Humber and North Yorkshire ICB - 03H | Humber and North Yorkshire ICB - 03K | Humber and North Yorkshire ICB - 03Q | Humber and North Yorkshire ICB - 42D |
|---|---|---|---|---|---|---|---|---|---|
Epilepsy: QOF prevalence (Persons 18+ yrs) | 2024/25 | 0.8 | 0.9 | 1.0 | 1.0 | 1.1 | 1.0 | 0.7 | 0.9 |
| Indicator | Period | England | NHS Humber and North Yorkshire Integrated Care Board - QOQ | Humber and North Yorkshire ICB - 02Y | Humber and North Yorkshire ICB - 03F | Humber and North Yorkshire ICB - 03H | Humber and North Yorkshire ICB - 03K | Humber and North Yorkshire ICB - 03Q | Humber and North Yorkshire ICB - 42D |
|---|---|---|---|---|---|---|---|---|---|
Epilepsy: QOF prevalence (Persons 18+ yrs) | 2024/25 | 0.8 | 0.9 | 1.0 | 1.0 | 1.1 | 1.0 | 0.7 | 0.9 |
There were 2,608 patients aged 18+ years who were diagnosed with epilepsy among Hull patients in 2024/25.
The percentage has remained relatively constant in Hull over the last few years as it has across the Humber and North Yorkshire Integrated Care Board and England, although the percentage in Hull has been consistently higher than both the Humber and North Yorkshire Integrated Care Board average and England.
Compared with benchmark
Epilepsy: QOF prevalence (Persons 18+ yrs)
|
Period
|
Humber and North Yorkshire ICB - 03F |
NHS Humber and North Yorkshire Integrated Care Board - QOQ
|
England
|
||||
|---|---|---|---|---|---|---|---|
|
Count
|
Value
|
95%
Lower CI |
95%
Upper CI |
||||
| 2009/10 | • | 1306 | 1.0% | 0.9% | 1.0% | 0.8% | 0.8% |
| 2010/11 | • | 1357 | 1.0% | 1.0% | 1.1% | 0.8% | 0.8% |
| 2011/12 | • | 1416 | 1.0% | 1.0% | 1.1% | 0.8% | 0.8% |
| 2012/13 | • | 2368 | 1.0% | 1.0% | 1.1% | 0.9% | 0.8% |
| 2013/14 | • | 2419 | 1.1% | 1.0% | 1.1% | 0.9% | 0.8% |
| 2014/15 | • | 2473 | 1.1% | 1.0% | 1.1% | 0.9% | 0.8% |
| 2015/16 | • | 2528 | 1.1% | 1.0% | 1.1% | 0.9% | 0.8% |
| 2016/17 | • | 2587 | 1.1% | 1.0% | 1.1% | 0.9% | 0.8% |
| 2017/18 | • | 2603 | 1.1% | 1.1% | 1.1% | 0.9% | 0.8% |
| 2018/19 | • | 2590 | 1.1% | 1.1% | 1.1% | 0.9% | 0.8% |
| 2019/20 | • | 2606 | 1.1% | 1.1% | 1.1% | 0.9% | 0.8% |
| 2020/21 | • | 2582 | 1.1% | 1.0% | 1.1% | 0.9% | 0.8% |
| 2021/22 | • | 2561 | 1.1% | 1.0% | 1.1% | 0.9% | 0.8% |
| 2022/23 | • | 2639 | 1.1% | 1.0% | 1.1% | 0.9% | 0.8% |
| 2023/24 | • | 2652 | 1.1% | 1.0% | 1.1% | 0.9% | 0.8% |
| 2024/25 | • | 2608 | 1.0% | 1.0% | 1.1% | 0.9% | 0.8% |
Source: NHS England
From the local analysis of the national Quality and Outcomes Framework datasets, there was no statistically significant association between the prevalence of diagnosed epilepsy and the average age of the practice patients across the 25 practices in Hull for 2024/25.
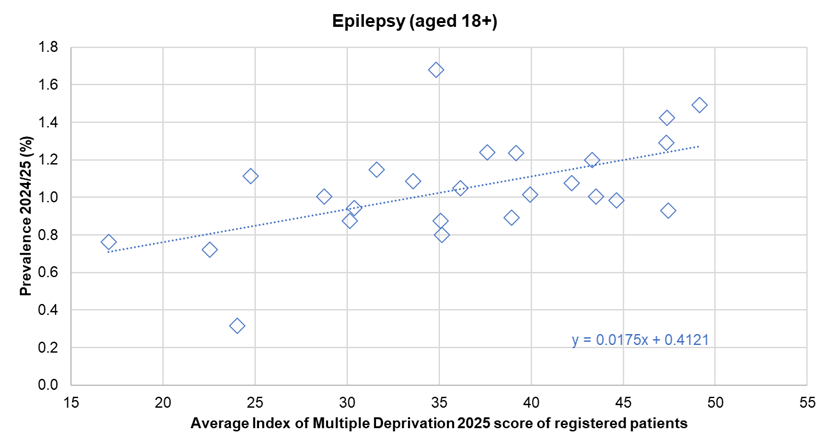
There was a statistically significant association between the prevalence of diagnosed epilepsy and the average deprivation score of registered patients (using the Index of Multiple Deprivation 2025) across the 25 practices for 2024/25. If the practices were divided into five approximately equal sized groups based on average deprivation score of patients (with each fifth having approximately one-fifth of the total registered patients in Hull) then the prevalence increased from 0.8% for the practices serving the patients living in the least deprived areas of Hull to 1.2% for the practices serving the patients living in the most deprived areas of Hull. For every 10 point increase in the average deprivation score of patients, the prevalence of epilepsy increased by 0.2 percentage points. Further analysis of diagnosed disease by the average deprivation score of practice patients is within the file within Local Analysis of Quality and Outcomes Framework Data.
Hospital Admissions
The number of hospital admissions for epilepsy per 100,000 population in Hull was 37% higher than England during 2023/24 among under 19s.
There was wide variation in the admission rate for epilepsy among under 19s across other local authorities within the region.
Compared with benchmark
| Indicator | Period | England | Yorkshire and the Humber region (statistical) | Kingston upon Hull | East Riding of Yorkshire | North East Lincolnshire | North Lincolnshire | York | North Yorkshire UA | Barnsley | Doncaster | Rotherham | Sheffield | Bradford | Calderdale | Kirklees | Leeds | Wakefield |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
Hospital admissions for epilepsy (under 19 years) (Persons 0-18 yrs) | 2023/24 | 79.3 | 98.6 | 108.7 | 76.0 | 99.7 | 192.9 | 147.1 | 205.7 | 121.0 | 100.4 | 73.6 | 41.2 | 103.8 | 73.6 | 86.3 | 46.1 | 106.5 |
| Indicator | Period | England | Yorkshire and the Humber region (statistical) | Kingston upon Hull | East Riding of Yorkshire | North East Lincolnshire | North Lincolnshire | York | North Yorkshire UA | Barnsley | Doncaster | Rotherham | Sheffield | Bradford | Calderdale | Kirklees | Leeds | Wakefield |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
Hospital admissions for epilepsy (under 19 years) (Persons 0-18 yrs) | 2023/24 | 79.3 | 98.6 | 108.7 | 76.0 | 99.7 | 192.9 | 147.1 | 205.7 | 121.0 | 100.4 | 73.6 | 41.2 | 103.8 | 73.6 | 86.3 | 46.1 | 106.5 |
The rate of hospital admission for epilepsy among under 18s in Hull has decreased from a high around 170 admissions per 100,000 population for 2013/14 and 2014/15, but there has been year-on-year variability due to the relatively small number of admissions.
With the exception of 2018/19 and 2020/21, the admission rate in Hull has been statistically significantly higher than England.
There were 70 admissions for epilepsy among Hull residents aged under 18 years in 2023/24. It is possible that some of these admissions could be among the same individuals (admitted more than once during the year).
Compared with benchmark
Hospital admissions for epilepsy (under 19 years) (Persons 0-18 yrs)
|
Period
|
Kingston upon Hull |
Yorkshire and the Humber region (statistical)
|
England
|
||||
|---|---|---|---|---|---|---|---|
|
Count
|
Value
|
95%
Lower CI |
95%
Upper CI |
||||
| 2013/14 | • | 100 | 169.7 | 135.0 | 202.7 | 88.6 | 77.8 |
| 2014/15 | • | 105 | 177.0 | 146.3 | 216.2 | 78.9 | 75.0 |
| 2015/16 | • | 75 | 125.6 | 95.8 | 153.7 | 81.7 | 77.1 |
| 2016/17 | • | 80 | 132.7 | 108.2 | 168.9 | 74.9 | 72.8 |
| 2017/18 | • | 70 | 115.4 | 87.1 | 142.1 | 76.8 | 73.5 |
| 2018/19 | • | 55 | 90.2 | 69.4 | 119.3 | 83.9 | 77.9 |
| 2019/20 | • | 75 | 121.8 | 97.2 | 154.5 | 84.2 | 79.6 |
| 2020/21 | • | 50 | 80.7 | 58.5 | 104.6 | 70.6 | 67.1 |
| 2021/22 | • | 75 | 121.1 | 95.2 | 151.8 | 80.6 | 73.5 |
| 2022/23 | • | 70 | 111.0 | 87.9 | 142.0 | 82.7 | 74.0 |
| 2023/24 | • | 70 | 108.7 | 84.7 | 137.3 | 98.6 | 79.3 |
Source: OHID, based on NHS England and Office for National Statistics data
Over the five year period 2020/21 to 2024/25, there were 1,420 admissions to Hull patients where the primary cause of the admission was epilepsy (numbers rounded to the nearest 5). There were around 300 each year for 2021/22 (290), 2022/23 (290) and 2023/24 (315) with slightly fewer in 2020/21 likely associated with the COVID-19 pandemic (255) and slightly fewer in the latest year 2024/25 (270).
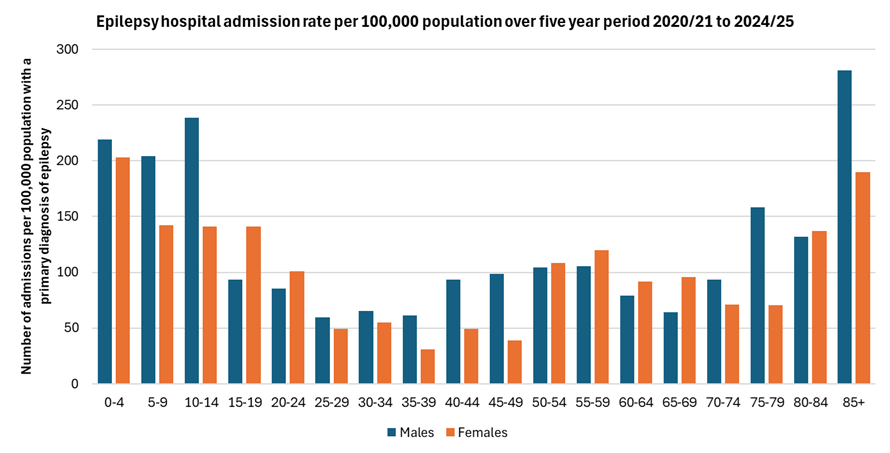
There were more males admitted compared to females over the five year period (775 versus 645). More men were admitted compared to women for each five year age group except for 15-24 years, 55-69 years, 80-84 years and 90+ years. The men who were admitted for epilepsy had a slightly lower average age compared to women (33.9 versus 35.8 years).
The table below shows the number of males and females admitted to hospital with a primary diagnosis of epilepsy over the five year period 2020/21 to 2024/25 by age (rounded to the nearest 5).
Some patients will be admitted to hospital more than once over the five year period.
| Age group | Males Total admissions | Females Total admissions | Persons Total admissions |
| 0-4 | 90 | 80 | 165 |
| 5-9 | 90 | 60 | 150 |
| 10-14 | 105 | 60 | 160 |
| 15-19 | 40 | 55 | 95 |
| 20-24 | 40 | 45 | 85 |
| 25-29 | 30 | 25 | 55 |
| 30-34 | 35 | 30 | 65 |
| 35-39 | 30 | 15 | 45 |
| 40-44 | 40 | 20 | 60 |
| 45-49 | 40 | 15 | 55 |
| 50-54 | 45 | 45 | 90 |
| 55-59 | 45 | 50 | 95 |
| 60-64 | 30 | 35 | 65 |
| 65-69 | 20 | 30 | 50 |
| 70-74 | 25 | 20 | 50 |
| 75-79 | 30 | 15 | 45 |
| 80-84 | 15 | 20 | 35 |
| 85+ | 25 | 30 | 55 |
| Total | 775 | 645 | 1,420 |
This work uses data provided by patients and collected by the NHS as part of their care and support.
The admission rates per 100,000 population are much higher among children particularly males aged under 15 years and people aged 80+ years. People in their 50s also had slightly higher rates compared to ages 20-74 years.
Some patients will be admitted to hospital more than once over the five year period.
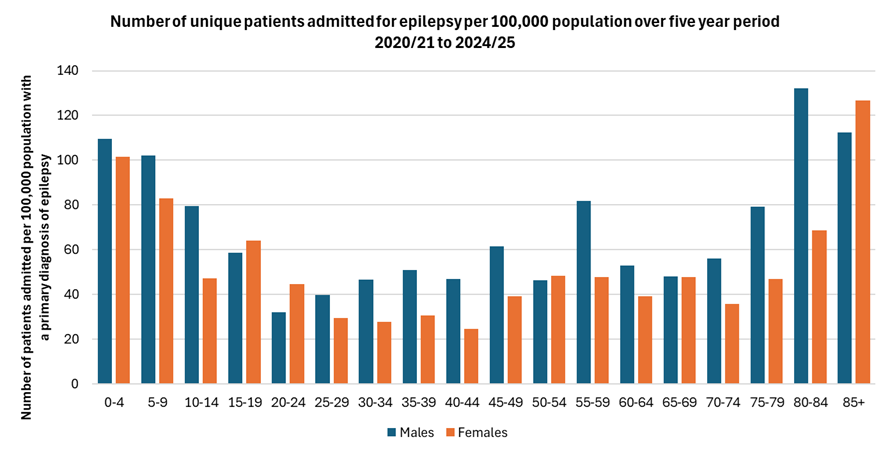
There were 755 patients in total who were admitted at least once with a primary diagnosis of epilepsy over the five year period. Almost two-thirds had a single admission with 490 (65%) admitted once, 135 (18%) admitted twice, 60 (7.9%) admitted three times, 20 (2.6%) admitted four times, 20 (2.6%) admitted five times, and 30 (4.0%) were admitted on six or more occasions over the five year period.
| Age group | Males Total admissions | Females Total admissions | Persons Total admissions |
| 0-4 | 45 | 40 | 85 |
| 5-9 | 45 | 35 | 80 |
| 10-14 | 35 | 20 | 55 |
| 15-19 | 25 | 25 | 50 |
| 20-24 | 15 | 20 | 35 |
| 25-29 | 20 | 15 | 35 |
| 30-34 | 25 | 15 | 45 |
| 35-39 | 25 | 15 | 35 |
| 40-44 | 20 | 10 | 30 |
| 45-49 | 25 | 15 | 35 |
| 50-54 | 20 | 20 | 40 |
| 55-59 | 35 | 20 | 55 |
| 60-64 | 20 | 15 | 35 |
| 65-69 | 15 | 15 | 30 |
| 70-74 | 15 | 10 | 30 |
| 75-79 | 15 | 10 | 30 |
| 80-84 | 15 | 10 | 25 |
| 85+ | 10 | 20 | 30 |
| Total | 425 | 330 | 755 |
This work uses data provided by patients and collected by the NHS as part of their care and support.
The number of unique patients admitted for epilepsy per 100,000 population is highest for children under 10 years, men aged 80+ years and women aged 85+ years. The number of admissions among men increased from age 20-24 years to 55-59 years but fell for those aged 60-64 years.
Mortality
The number of deaths where epilepsy is the underlying cause of death is relatively small. Over the five year period 2021 to 2025, there were 35 deaths in total with six in ten of them among males (21) and four in ten among females (14). All deaths were among adults and ranged from 20 to 90 years for the five year period.
Among men, the average age at deaths 52.2 years among those dying of epilepsy. There were eight deaths among men aged 20-39 years, four deaths among men aged 40-59 years, seven deaths among men aged 60-79 years and two deaths among men aged 80+ years.
Among women, the average age at deaths 71.1 years among those dying of epilepsy. There were four deaths among women aged under 60 years, three deaths among women aged 60-79 years and seven deaths among women aged 80+ years.
Strategic Need and Service Provision
It is important that people who have a seizure for the first time seek emergency treatment, and for people with diagnose epilepsy do not miss epilepsy medicine, attend their health reviews and have a care plan in place.
People with epilepsy should make sure friends and family know what to do if a person has a seizure. It is also advisable that people with epilepsy wear a bracelet or carry a card to let people know they have epilepsy. It is useful if people with epilepsy keep a diary to help identify factors that might trigger a seizure such as tiredness, stress, menstruation, flashing lights, food or drink. Homes can also be made safer by having fitted carpets and radiator covers.
It is also necessary to think about safety when doing activities like cooking, using tools or machinery, swimming or sport, and consider having showers instead of baths. Anyone who had had any type of seizure should not drive, and must tell the Driving Vehicle and Licensing Agency (DVLA). When a person can start driving again depends on the type of seizure and when it last happened. There are DVLA rules in place about epilepsy and driving which must be followed.
Resources
NHS. Epilepsy. Epilepsy – NHS
The Office for Health Improvement & Disparities’ Fingertips: https://fingertips.phe.org.uk/
Updates
This page was last updated / checked on 25 March 2026.
This page is due to be updated / checked in August 2026.